A quality collaborative on Kendall Regional Medical Center to reduce the door-to-balloon time in STEMI patients is the issue for consideration in the paper. Several steps led to the development of this issue including the necessity to help and provide STEMI patients with treatment in a short period, the investigations and the discovery of the possibility to reduce the D2B time, and the comparison of the averages at the state and national levels (Wilson et al., 2013). However, such issues as staff’s poor awareness of all their duties, the necessity to report all the time, poorly developed checklists, and transport delays cannot be ignored (Miedema et al., 2011). Therefore, such preventive steps as cross-training, the analysis of causes of transport delays, and the implementation of the Lean Six Sigma methodology could be offered at the medical center (Ellahham, Aljabbari, Mananghaya, Raji, & Zubai, 2015).
The success of the analysis of the process threats is based on the appropriate incorporation of strengths, weaknesses, opportunities, and threats of the issue under consideration. The reduction of the D2B time in STEMI patients is the quality issue that is based on the following aspects:
- Strengths: a proved possible to reduce the door-to-ECG time (Coyne et al., 2015), the development of special techniques to reduce the time, and the desire of the staff to be trained, communicated, and share personal experience;
- Weaknesses: poorly developed emergency room and equipment, not always available Cath Labs, and the inability to avoid a human factor;
- Opportunities: communication with patients, the analysis of patient-reported outcome measures (Frosch, 2015), and the improvement of STEMI patients’ outcomes;
- Threats: inabilities to structure a working process and the uncertainty of the readiness of all medical workers to cooperate.
For example, the investigations of Shiomi and the team (2012) proved that teamwork and cooperation could be used to reduce the D2B time and improve the quality of primary help offered to STEMI patients. However, the results of the study show that the steps cannot be predicted and guarantee 100% success. Therefore, it is necessary to think about additional steps to reduce the D2B time.
The idea to use a fishbone diagram and investigate the causes and effects that led to the quality issue could be offered.
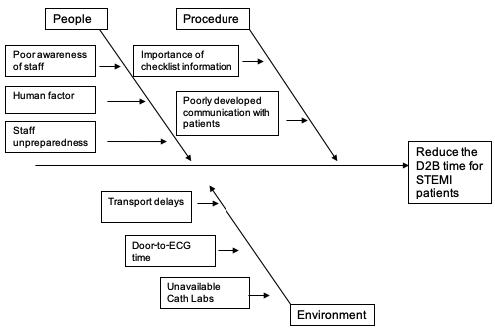
The investigations of Coyne et al. (2015) contribute to the field of healthcare and nursing considerably because they introduce the idea to improve the door-to-ECG time for STEMI patients as the only possible way to reduce the D2B time.
The main similarity of the present approach in the form of the fishbone diagram and past research is the goal established by researchers. The projects aim at developing special programs and steps to reduce the D2B time and provide STEMI patients with fast and high-quality help. The differences between the approaches are the orientation of the steps. In the current study, it is necessary to identify and comprehend the causes of the problem and the steps that led to the creation of the quality issue. Past research aimed at evaluating the steps that could help the staff to change the working process.
The offered tool is effective due to the possibility to focus on the organizational issues, personal factors, and the contributions that could be made by people and the technologies they use. The diagram shows that the necessity to reduce the D2B time has its roots. Therefore, the problem could be solved.
References
Coyne, C.J., Testa, N., Desai, S., Lagrone, J., Chang, R., Zheng, L., & Kim, H. (2015). Improving door-to-balloon time by decreasing the door-to-ECG time for walk-in STEMI patients. Western Journal of Emergency Medicine, 16(1), 184-189.
Ellahham, S., Aljabbari, S., Mananghaya, H., Raji, J., & Zubai, A. (2015). Reducing door-to-balloon time for acute ST-elevation myocardial infarction in primary percutaneous intervention: Transformation using robust performance improvement. BMJ Quality Improvement Reports, 8(4), 1-4.
Frosch, D.L. (2015). Patient-reported outcomes as a measure of healthcare quality. Journal of General Internal Medicine, 30(10), 1383-1384.
Miedema, M.D., Newell, M.C., Duval, S., Garberich, R.F., Handran, C.B., Larson, D.M., Mulder, S., Wang, Y.L., Lips, D.L., & Henry, T.D. (2011). Causes of delay and associated mortality in patients transferred with ST-segment-elevation myocardial infarction. Circulation, 124, 1636-1644.
Shiomi, H., Nakagawa, Y., Morimoto, T., Furukawa, Y., Nakano, A., Shirai, S.…Kimura, T. (2012). Association of onset to balloon and door to balloon time with long-term clinical outcome in patients with ST-elevation acute myocardial infarction having primary percutaneous coronary intervention: observational study. BMJ, 344, 1-14.
Wilson, B. H., Humphrey, A. D., Cedarholm, J. C., Downey, W. E., Haber, R. H., Kowalchuk, G. J., Garvey, L. (2013). Achieving sustainable first door-to-balloon times of 90 minutes for regional transfer ST-segment elevation myocardial infarction. Journal of American Cardiovascular Interventions, 6(10), 1.