Literature Review
This literature review focuses on significant issues in nurse-led interventions for the management of chronic illnesses. A central goal of chronic illness management is to support patient participation in self-care. Self-efficacy can be achieved through nurse interventions that involve health literacy programs geared towards improving functional capacity and self-management (Ades et al., 2013).
The quality of life (QOL) of elderly patients can be enhanced through activities that enhance their functional capacity. For example, it was suggested that QOL of patients with CHF could be improved through training on Tai Chi meditation method (Sun, Buys, & Jayasinghe, 2014). The technique is not only effective in improving breathing and relaxation, but also supports the management of blood pressure and BMI in elderly CHF patients (Sun et al., 2014).
Exercise therapy (30-minute sessions, four times a week) has been shown to increase QOL of elderly patients and reduces depression (Ades et al., 2013). Further, exercise routine is a component of cardiac rehabilitation interventions that helps reduce re-hospitalization rates for CHF patients. Other techniques for improving functional capacity include dancing therapy and health education to foster self-care and improve healthcare resource utilization by the elderly (Ades et al., 2013). Chronic illnesses are associated with poor patient outcomes and QOL.
Studies agree that nurse-led patient education increases patient confidence in self-management. Health teaching on self-care skills, e.g., daily caloric intake, symptom identification, and prescription adherence, reduces re-hospitalizations and ED admissions (Sun et al., 2014). Enhanced self-management comprehension or self-care efficacy can be achieved through “face-to-face communication, telephone counseling, or E-learning programs” (Sun et al., 2014, p. 293). These nursing interventions improve patient confidence and skills in self-care to enhance medication adherence and outcomes.
Studies have examined e-health as an essential approach for improving patient engagement in self-management. They included an evaluation of an e-learning program for CAD patients that comprised an educational site with informational resources for patients and an interactive platform for seeking expert advice (Salameh, Gomaa, El-Senousy, & Salameh, 2012).
The results indicated improved physical, psychological, and social functioning as well as elevated QOL. Thus, the e-learning approach can support health education by allowing patients to express their concerns and establish supportive relationships. Another study suggests that nursing education improves four QOL domains – “activity tolerance, self-management, lifestyle modification, and medication compliance” (Samaritiz, Dimopoulos, Tziongourou, & Nanas, 2013, p. 130). Therefore, health teaching by nurses can increase patient comprehension of self-management, resulting in QOL improvements.
Chronic illnesses, e.g., CHF, are associated with poor QOL in the elderly population (Bulter, 2012). Therefore, nursing interventions that improve QOL of the vulnerable population are critical in rehabilitative care. For instance, nurses caring for patients with heart conditions can teach the Tai Chi technique or physical training as part of the cardiac rehabilitation program (Ades et al., 2013).
Evidence shows that these activities enhance physiological functioning, lower BP, and improve cardiac function, which result in elevated QOL (Bulter, 2012). The other important nursing intervention is psychosocial support to minimize mental/emotional distress. Effective communication methods enhance the efficacy of health teaching to the patients. Advanced technology, e.g., e learning, can bolster self-monitoring, self-management, and lifestyle changes due to improved comprehension, interactivity, and support (Bulter, 2012).
Methodology and Design of the Study
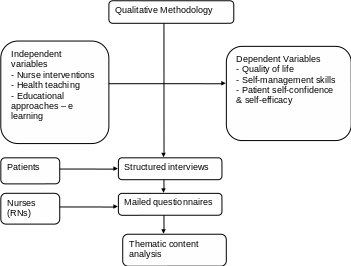
The primary purpose of this research is to determine the way a nurse might contribute to the improvement of the health of patients suffering from chronic diseases. To achieve this aim, a qualitative approach will be used to explore the nurses’ perceptions and experiences with chronically ill patients. The qualitative approach is the most appropriate methodology because the study involves an exploration of key variables – nurses’ perceptions/views on interventions, specific educational approaches, and nursing role in caring for chronically ill elderly patients.
Further, through a qualitative methodology, the researcher can examine participant views within a clinical context (Polit & Beck, 2012). In this research, a qualitative study design will be employed. It will involve obtaining the subjective experiences of the participants on the issue of health teaching of patients to enhance comprehension and outcomes. According to Polit and Beck (2012), a qualitative study design is essential in uncovering and interpreting participant views to develop concepts/theories about a topic of interest.
Data collection will involve semi-structured interviews performed in the patients’ homes and questionnaires mailed to RNs. Polit and Beck (2012) state that semi-structured interviews have the benefits of specificity and contextualization of issues. They also give room for follow-up answers. The two instruments will help uncover themes from verbatim reports and Likert scale items. Data analysis will involve thematic content analysis of coded responses to facilitate valid interpretations of the qualitative data – attitudes and views of patients/nurses on health education.
Sampling Methodology
The study will use a purposive sampling technique to recruit participants. Purposive sampling entails selecting the most representative and knowledgeable individuals to take part in a study (Polit & Beck, 2012). The target population will be RNs and patients suffering from chronic illnesses. For the nurse participants, the inclusion criteria are RNs and over 1-year experience caring for chronically ill elderly patients. In contrast, the patients included will be those with long-term illnesses (asthma, diabetes, cancer, CAD, etc.), elderly males and females, ready to share their experiences/views, and interacting regularly with nurses.
Participant recruitment will involve RNs working in long-term care facilities for the elderly. They will receive written information – aims and design – concerning the research to help facilitate the recruitment process. Similarly, the participants will receive the same information prior to recruitment. Additional ethical considerations will include informing the respondents that they can withdraw from the research at any time without permission and informed consent (Polit & Beck, 2012). Further, the confidentiality of the participants will be ensured using codes during the interviews. The interviews will also be conducted in the participants’ homes to guarantee confidentiality and anonymity.
For the patients, the interviews will focus on the experiences of the patients with health education and its efficacy in self-management. Additionally, their healthcare encounters will be examined to obtain a wider perspective on the nursing role in patient education. The purposive sampling technique is aimed at recruiting information-rich subjects with a deeper understanding of the topic (Polit & Beck, 2012). An appropriate sample size will be based on information power. The concept of information power holds that if the participants can give quality information about the topic, then a small sample size is enough to achieve data saturation (Polit & Beck, 2012). As such, the sample size will be 27 RNs and 10 patients with chronic illnesses. The rationale for selecting a large number of nurses is that response rates rarely reach 100%. The respondents will differ widely in age, gender, and disease (patients) to receive a broader perspective on the topic.
Necessary Tools
Interview Form
Semi-structured interviews will involve forms with questions for the participants. Polit and Beck (2012) note that semi-structured interviews contain a set of specific “themes and questions” and allows flexibility in questioning to obtain follow-up responses (p. 78). In this study, they will be structured to cover the key variables captured in the research questions – interventions, health education impact, health teaching approaches, and nursing role. The patients will be asked various questions in a 30-minute interview. Examples include; how would you describe your encounter with nurses and health teaching? What do you consider effective patient education methods to be? Can you give examples? After the interviews, verbatim records will be transcribed for analysis.
Questionnaire
A pretested questionnaire instrument will be used in the survey of nurses (RNs). The questionnaires will be mailed to eligible participants who will return them to the researcher upon completion. The first part of the questionnaire will capture the demographic details of the participants, including age, gender, and years of experience. The questions/items will be structured around 5-point Likert scale to facilitate analysis. The key themes in the questionnaire will be self-care education for chronically ill elderly patients, experience with health teaching, and interventions implemented. The aim is to understand the nurses’ perspectives on the efficacy of interventions and health education in improving the QOL of patients with chronic illnesses.
References
Ades, P., Keteyian, S., Balady, G., Houston-Miller, N., Kitzman, D., Mancini, D., & Rich, M. (2013). Cardiac rehabilitation exercise and self-care for chronic heart failure. JACC Heart Failure, 1(6) 540-547. doi:10.1016/j.jchf.2013.09.002.
Bulter, J. (2012). Primary prevention of heart failure. International Scholarly Research Network, 1(1), 1-16. doi:10.5402/2012/982417
Polit, D. F., & Beck, C. T. (2012). Nursing research: Generating and accessing evidence for nursing practice. Philadelphia: Lippincott Williams and Wilkins.
Salameh, B., Gomaa, N., El-Senousy, T., & Salameh, O. (2012). Effect of an e-learning program on the quality of life of patients with coronary heart disease. Procedia – Social and Behavioral Science, 55, 284-293.
Samaritiz, L., Dimopoulos, S., Tziongourou, M., & Nanas, S. (2013). Effects of psycho-social interventions on quality of life in patients with chronic heart failure: A meta-analysis of random control trials. Journal of Cardiac Failure, 19(2), 125-134. doi:10.1016/j.cardfail.2012.12.004
Sun, J., Buys, N., & Jayasinghe, R. (2014). Effect of community-based meditative Tai Chi program on improving quality of life, physical and mental health in chronic heart failure participants. Aging and mental health, 18(3), 289-295. doi: 10.1080/13607863.2013.875120