Introduction
Asthma is a chronic airway disease that has a considerable impact on the population health of the US. According to Loftus and Wise (2016), 8.6% of people in the US have asthma in comparison with 4.3% worldwide. Moreover, the prevalence of the disease is increasing both in the US and worldwide, which has considerable implications, especially for lower socioeconomic populations (Loftus & Wise, 2016). The present paper offers an overview of the condition and provides information about the possible pharmacological and non-pharmacological treatments and interventions to address the problems associated with the disease.
Pathophysiology, Risk Factors, Signs and Symptoms
Asthma is a condition that is associated with wheezing, breathlessness, chest tightness, and cough due to air hyper-responsiveness (Bush, 2019). These symptoms are usually associated with airflow obstruction, which can be reversed with treatment or spontaneously (Bush, 2019). Asthma is associated with airways inflammations, which tighten the airway smooth muscles by thickening the walls (Bush, 2019).
It may also lead to an increase in mucus-secreting cells and loss of enzymes. The environmental risk factors of asthma include smoking, pollution, obesity, exposure to microbes, stress, and genetics (Toskala, & Kennedy, 2015). Moreover, according to Loftus and Wise (2016), asthma is more common in children (9.7%) than in adults (7.7%). In other words, the pathophysiology of the condition is complex, and risk factors are numerous.
Health Promotion
While the condition is highly prevalent worldwide, the evidence concerning efficient ways of preventing diseases is limited. According to Beasley, Semprini, and Mitchell (2015), the primary preventative measure should be aimed at reducing environmental factors, such as tobacco smoking, obesity, indoor and outdoor pollution, promoting breastfeeding, and reducing social inequality. Additionally, adults with a high risk of asthma are to undergo routine screening for asthma using specialized questionnaires, such as the nine-item tool promoted by Yadollahzadeh et al. (2019). The primary way of maintenance is avoiding environmental triggers, taking prescribed medicine, and knowing when asthma is getting worse and how to manage the complications (Beasley, 2015). In short, health promotion strategies are dictated by identified risk factors and the absence of sufficient evidence for efficient prevention.
Independent Nursing Interventions
Independent nursing interventions usually include assessments, therapy, and education. Nurses are to assess patient history, medication regimen, and respiratory status (Ramsay, Schwindt, Nguyen, & Margellos-Anast, 2018). Nurses are also expected to provide patient education concerning risk factors, self-assessment, and non-pharmacological management techniques (Ramsay et al., 2018). Patient education is to be adapted depending on the age and literacy level of patients to adhere to ethical standards and improve adherence to preventative measures. Moreover, nurses should administer prescribed medications and fluids and monitor patient’s responses to treatment (Ramsay et al., 2018). In short, nurses are to facilitate the work of physicians and promote self-care strategies.
Diagnostics
The diagnosis of asthma is a challenging process because it is associated with ruling out conditions that have similar signs, including chronic obstructive pulmonary disease (COPD). The diagnosis procedure usually consists of assessing history for possible risk factors, physical examination, together with spirometry and peak flow analysis (McCracken, Veeranki, Ameredes, & Calhoun, 2017). Additional tests may include X-ray and high-resolution computerized tomography (CT), nitric oxide test, allergy testing, and methacholine challenge (McCracken et al., 2017). The diagnosis is not always self-evident due to the presence of diseases with similar representation.
Pharmacologic Treatments
Pharmacologic treatment is classified into long-term asthma control medications and quick-relief medications for emergencies. The long-term medications include inhaled corticosteroids, leukotriene modifiers, long-acting beta-agonists, combination inhalers, and theophylline (McCracken et al., 2017). These medications aim at controlling inflammation and preventing airways from tightening. The rescue medications are needed to provide immediate relief when the airway walls thicken so that air cannot pass freely. Such medications include short-acting beta-agonists, ipratropium, and oral or intravenous corticosteroids (McCracken et al., 2017). Since there is no cure from the disease, pharmacologic treatment aims at controlling symptoms.
Nursing Diagnoses & Priority Concepts
As discussed in the nursing intervention section, nursing diagnosis consists of various assessments. Nurses are to evaluate the effectiveness of the breathing pattern related to swelling and spasm of the bronchial tubes, which may be witnessed during physical activity (Ramsay et al., 2018). Nurses should also make sure that the patient understands the treatment plan and determine if there are any quality of life issues connected with the treatment that can be improved.
Additionally, nurses are expected to identify if patients are aware of medication administration procedures, such as the use of inhalers and oral medication intake regimen (Ramsay et al., 2018). The nursing diagnosis process also includes identifying if patients understand emergency measures and standard treatment. In short, a nursing diagnosis is a basis for further independent nursing interventions
Conclusion
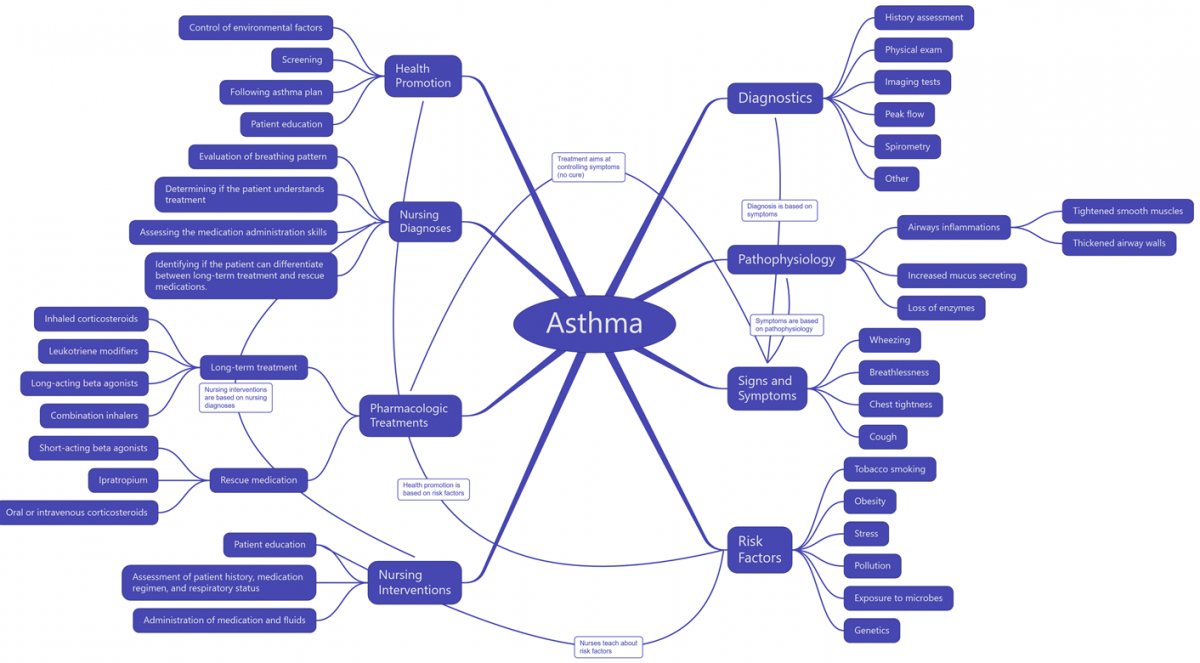
Asthma is a complicated concept that is to be understood in its entirety to improve patient outcomes. The concept includes pathophysiology, risk factors, signs and symptoms, health promotion, diagnostics, nursing diagnoses and interventions, and pharmacologic treatments. However, visualization of the matter may be advantageous for understanding the matter. Figure 1 below is an example of the concept map for asthma.
References
Beasley, R., Semprini, A., & Mitchell, E. A. (2015). Risk factors for asthma: is prevention possible? The Lancet, 386(9998), 1075-1085.
Bush, A. (2019). Pathophysiological mechanisms of asthma. Frontiers in Pediatrics, 7, 1-17.
Loftus, P. A., & Wise, S. K. (2016). Epidemiology of asthma. Current opinion in otolaryngology & head and neck surgery, 24(3), 245-249.
McCracken, J. L., Veeranki, S. P., Ameredes, B. T., & Calhoun, W. J. (2017). Diagnosis and management of asthma in adults: A review. JAMA, 318(3), 279-290.
Ramsay, J., Schwindt, T., Nguyen, T., & Margellos-Anast, H. (2018). Translating a proven pediatric healthy homes asthma intervention to adults. Health Promotion Practice, 19(2), 222-232.
Toskala, E., & Kennedy, D. (2015). Asthma risk factors. International Forum of Allergy & Rhinology, 5(S1), S11-S16. Web.
Yadollahzadeh, M., Hashemian, S., Kiani, A., Ghorbani, F., Najafizadeh, K., Razavi, F., & Abedini, A. (2019). Diagnostic values of bronchodilator response versus 9-question questionnaire for asthma. Advances in Respiratory Medicine, 87(5), 269-275. Web.