Objective
This study has been conducted to know what differences are there in education through high ranked university and low ranked university? In this study, attempt has been made to explain how much the low ranked university have to be upgraded to reach the same level of high ranked university. Charts and tables are used to show the ranks of the universities. Survey has been used as a data collection apparatus to assemble information in a row about persons. Surveys are collecting of data which are used to reveal something psychologically. Survey should be able to determine concepts. “Indian Universities are supported and funded by University Grants Commission (UGC). UGC also provides recognition to the universities in India through National Assessment and Accreditation Council (NAAC). There are some open universities in India providing courses through, correspondence and distance learning education mode” (List of Top Universities in India, Best Ranking Indian University, University List in India, Best Universities in India, 2010).
This study attempts to reveal the conditions of different universities through statistical approach. In India, universities are under the guidance of National Assessment and Accreditation Council (NAAC), which is a legally recognized organization by the UGC in September 1994. It is located at Bangalore and its primary role is to weigh up the presentation of the Universities. ”NAAC is based on objective and continuous improvement rather than being punitive or judgmental, so that all institutions of higher learning are empowered to maximize their resources, opportunities and capabilities” (National Assessment and Accreditation Council).
In this study, data collection method has been used which is a most familiar one. This means the researcher has collected data from secondary sources and through web search etc. “The B grade ranking has thoroughly disappointed us. We are going for an appeal,” a visibly upset vice-chancellor Y R Haragopal Reddy said. Naac committee basically looks into curricular system, teaching, learning and research aspects, consultancy and extension, infrastructure, student support programme, governance and leadership and, finally, innovative practices to assess the performance of an educational institution” (Varsity Sees Foul Play in Poor Ranking).
Different types of ranking are there to assess the standard of universities. Shanghai ranking and Times ranking are the major systems. Here we use time ranking system. “If properly performed, most scientists would consider peer review to have very good construct validity; many may even consider it the gold standard for appraising excellence. However, even peers need some standardized input data to peer review. The Times simply asks each expert to list the 30 universities they regard as top institutions of their area without offering input data on any performance indicators” (Ioannidis).
Questionnaire
- What are the accesses in giving rank to universities?
- What are the facilities providing by the high ranked universities than low ranked universities?
- Which are the levels of university ranking?
- Are there known biases in this Ranking?
- Why the rank of universities does not go beyond the 6000th mark?
- What is the proof that the students from high ranked universities are highly qualified?
- What are the benefits enjoyed by to ranked university through NAAC recognition?
- Do the universities succeeded in improving their recognition after the ranking process?
- Are the students in high ranked universities satisfied?
- Which are the associations related with the ranking process?
For this study, seven of the top ranking universities in the world have been taken as samples and the graph drawn, which shows ranks of the university. Graph also shows in its x-axis universities name and in y-axis rank. The best performing university is that one which has lower rank.
High ranked universities:
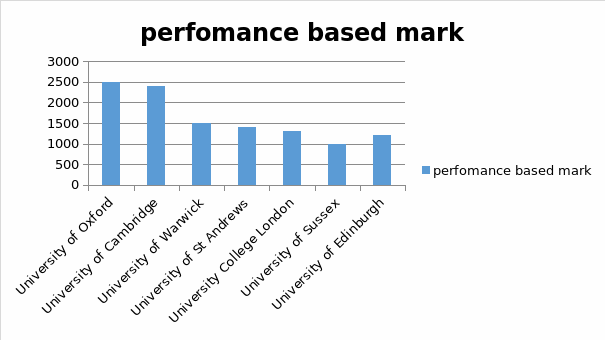
Low ranked universities
Since 2009, the rankings have been published by the Shanghai Ranking Consultancy (Academic Ranking of World Universities). A lot of other universities are there where there are no objection to provide admission but they are ranked very low. In case of those universities, performance does not become the factor to get admission. It is easy to get admission even though performance of the students is bad.
Low ranked universities are
- “University of North Alabama
- Wayne State University
- Virginia State University
- Troy University
- Brown University
- University of Alabama
- Florida International University
- Oklahoma State University
- Colorado State University
- Louisiana State University
- West Virginia University
- University of Cincinnati
- Stony Brook University
- San Diego State University
- Mississippi State University
- University of Central Florida
- Michigan Technological University
- Montana State University
- Clemson University
University of Idaho” (List of Low-Ranked Universities in USA).
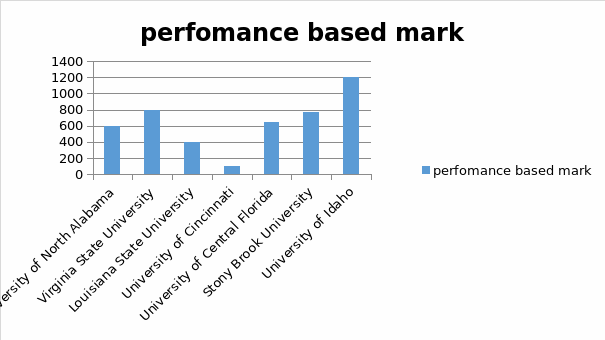
Observation
After completing the survey the study reveals that high ranked universities are more powerful than low ranked universities because those universities register high performance in all fields. “UT Southwestern Medical Center was ranked near the bottom of U.S. medical schools in how it fulfilled its “social mission,” particularly in how well it produced primary-care doctors, according to a study released Tuesday” (Jacobson). These universities will give more importance to practical application of education and besides they improve the extra curricular activity as they given the importance to the curriculum. “High-ranking programs include: atmospheric and oceanic sciences; applied mathematics; chemical engineering; Spanish; chemistry and biochemistry; geology; ecology and evolutionary biology; theatre; linguistics; neuroscience; and philosophy; molecular, cellular and developmental biology” (Anas).
There are also other universities which have high rank but not getting enough facility to students and they are over crowed at the time of admission. “Other first-class facilities at Newcastle include our library service, which is ranked as one of the top 10 in the world in the ISB survey” (Newcastle University).
Works Cited
Academic Ranking of World Universities. Wapedia. Web.
Anas, Brittany. Doctoral Programs at CU-Bolder Rank High in National Research Council Report. Daily Camera. 2010.
Ioannidis, John. et al. International Ranking System for Universities and Institutions: A Critical Appraisal. 2007. BMC Medicine.
Jacobson, Sherry. UT Southwestern Ranked Low in ‘Social Mission’ Study of Medical Schools Some Say is Flawed. Dallas News.Com. 2010. Web.
List of Low-Ranked Universities in USA. EduCouncil.Org. 2008. Web.
List of Top Universities in India, Best Ranking Indian University, University List in India, Best Universities in India, 2010. Infinite Coruses.Com. 2010.
National Assessment and Accreditation Council. University Grants Centres. 2007. Web.
Newcastle University. Top Universities. 2010. Web.
Ranking America’s Leading Universities on Their Success in Integrating African Americans. The Journal of Blacks in Higher Education. 2002. Web.
Varsity Sees Foul Play in Poor Ranking. The Times of India. 2010. Web.