Pain is a salient symptom for most conditions that are usually treated in the acute settings. Reasons for this pain are varied, and most patients prefer to endure their pain until they cannot put up with it any longer. The hospital environment does not seem to soothe patients, and, alongside with psychological and socioeconomic factors, pain management requires more than just drug administration. This purpose of this paper is to discuss the prevalence, assessment and management of pain in acute care hospital settings because there have been numerous misconceptions regarding this topic.
As treatment protocols advance and get better, there is a simultaneous increase in risks that compromise the general well-being of patients. Pain does not necessary mean physical pain; it also entails emotional pain, social distress and psychological pain. There is no scientific literature on the prevalence of acute pain, presumably because it is arduous to quantify pain as it occurs for all the different conditions. In addition, there is underreporting and under-diagnosis of pain. Pain is a critical sign among cancer patients, and it accounts for 53% for all the stages of cancer. It also prevails among dementia patients and surgical operations for various reasons. Such statistics is not accurate due to the high instances of underreporting and poor assessment. Patients are already engulfed with psychological pain and distress of the condition they are suffering from by the time they are visiting a hospital. In addition, patients do not wish to disclose their pain. In acute care settings, health care workers are charged with the responsibility of instilling confidence and security among the patients.
Health care professionals are mandated with the obligation to provide person-centered care in provision of positive and supportive interactions that create a feeling of value and involvement in their care. This interaction is perceived to be the first step in the assessment of pain in acute care settings. Doctors are biased towards this cause since they expect the patients to report the occurrence of pain as it occurs. Unfortunately, there are so many instances of underreporting because patients are not willing to say they are in pain unless it gets out of hand. A qualitative study by Choi et al. (2013, p. 67) indicates that doctors lack the proper resources that could aid in assessment of pain. For example, opioid use that may impede pain management efforts should be reviewed when taking histories so that effective management strategies are developed, but this does not happen. Pain assessment in older adults is a challenge because cognitive impairment leads to diminished ability to report pain, and caregivers’ ability to identify pain.
The management of pain in hospitals is jeopardized by various factors, among them being the attitude of the doctors. The table below indicates some of the misconceptions by the doctors in the management of pain among the elderly:

The qualitative study by Laitinen, Kaunonen, Astedt-Kurki (2011, p. 388-389) indicates that doctors and other health professionals operate under a compulsory timetable that makes them unapproachable due to their hastiness, creating a hostile environment. Nurses practices are task –oriented, and they operate under routine schedules of both direct and indirect nursing duties. Some patients will therefore prefer to stay in pain as long as it is manageable, and they avoid facing a hostile attitude from the staff. Person-centered interactions help in the management of emotional and psychological pain by talking with the patients about their diagnosis and required interventions. This interaction rarely exists; hence, the patients are not psychologically at peace and are socially isolated. The person-centered interaction creates a feeling of trust, respect and confidence within the patient.
Education is another factor that influences pain prevalence. Despite the fact that some news is usually bad, a study by Laitinen, Kaunonen, Astedt-Kurki (2011) indicated that being informed helped patients to gain control of their situation; hence managing their pain, subsequently reducing its prevalence. The study by McTier, Botti & Duke (2014) gives reasons for patient participation in pain management as follows:
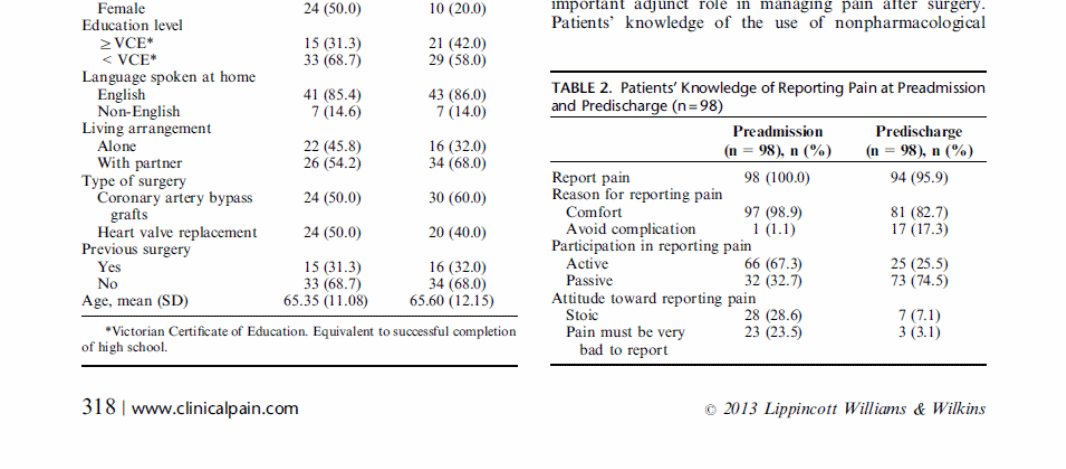
This table explicitly indicates that patients do not understand issues related to pain, and it is apparent that the doctors do little to create openness among the patients. Patients perceive pain management as an activity that entails the use of drugs only; hence, only doctors can make all the decisions pertaining to their pain. On the contrary there are also non-pharmacological approaches, shown below, that are as effective in the management of pain in acute care settings (McTier, Botti & Duke, 2013, p. 319).
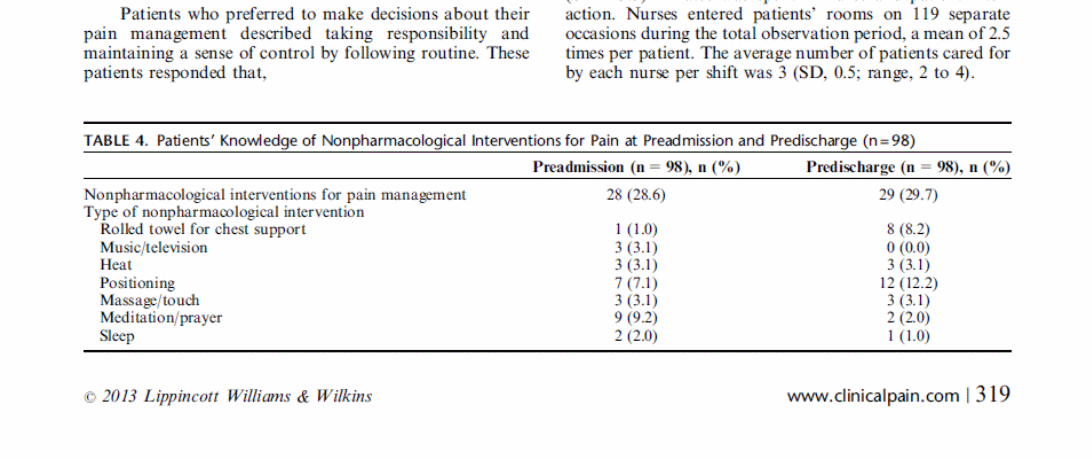
A study by Choi et al. (2013) indicates some sluggishness on the side of the nurses as indicated by low rates in the usage of pain assessment tools. This study aimed at devising ways of improving pain management in acute care settings in accordance with the JCI standards. The study was a cross-sectional study and collected qualitative information in determining gaps and barriers in pain management among cancer patients. This study identified a limitation in various areas such as education of evidence-based practice among nurses, pain management guidelines, documentation systems, information education and communication (IEC) materials and busy schedules for the nurses. Hence, the prevalence of pain in acute care settings continues to be high. Patients and caregivers expressed their fears of taking medication that was attributed to “fear of addiction and side effects, acknowledgement of higher level of pain and uncertainty about administration of the medicine” (Choi et al., 2013, p. 67). This was a peculiar finding as opposed to the belief that consistent use of drugs is helpful in pain management.
Despite the fact that different approaches in the management of pain prevail for the various conditions and ailments, education and creation of awareness for both the patients and the health care givers are imperative. McTier, Botti & Duke (2014) emphasize that creating awareness of pain and its management among patients is necessary to increase their participation in this endeavor. In this study, the nurses seem to rely solely on what the patients report and no tools are used to assess pain. Pain assessment tools are important to capture even those cases of pain that go unreported. A mere 25% of the pain assessments carried out in McTier, Botti & Duke’s (2014) study entailed the use of a mere rating scale in quantifying pain, indicating low usage of pain assessment tools. The environment, however, makes it difficult to use the pain assessment tools due to the task-oriented schedules that make it impossible for a client to be totally free with the doctors and nurses. Nurses spend less time (3.8 minutes out of 17.4 minutes spent in a patient’s room) interacting with patients; hence, restricting patient involvement (McTier, Botti & Duke’s, 2014, p. 319).
Some instances of pain manifestations are misunderstood by the doctors to mean destructive demeanor as is the case with dementia patients, whose ways of expressing pain may be unrecognizable. The table below indicates some of the attitudes of the doctors towards pain management in older adults. Pain management in older adults has been poorly managed due to misconceptions by both the patients and health workers. According to Newton, Reeves, West & Schofield (2014), pain is deemed a normal occurrence in older adults, while the adults think that the doctors and nurses are aware of the pain that they may be going through. Older adults, however, are reluctant to use analgesics to relieve pain, and, instead, prefer to use non-pharmacological approaches that would help them take part in managing their pain (Newton, Reeves, West & Schofield, 2014, p. 140).
Pain management is a comprehensive activity that requires the involvement of the patients, their caregivers and the health professionals. Reporting pain is the first step towards pain management, and in most cases, health professionals respond by giving pharmacological intervention. Depending on the cause of pain, nonpharmacological interventions also play an important role in the management of pain in acute care settings.
References
Choi, M., Kim, H. S., Chung, S., Ahn, M., Yoo, J., Park, O., …Oh, E. (2014). Evidence- based practice for pain management for cancer patients in an acute care setting. International Journal of Nursing Practice 20, 60-69.
Laitinen, H., Kaunonen, M., Astedt-Kurki, P. (2011). When time matters: The reality of patient care in acute care settings. International Journal of Nursing Practice, 17, 388-395.
McTier, L., Botti, M., & Duke, M. (2013). Patient participation in quality pain management during an acute care admission. Clin J Pain, 30, 316-323.
Newton, P., Reeves, R., West, E., & Schofield, P. (2014). Patient-centred assessment and management of pain for older adults with dementia in care home and acute settings. Reviews in Clinical Gerontology, 24, 139-144.