COPD as the Current Healthcare Concern
Chronic obstructive pulmonary disease (COPD) is a common issue that affects a significant number of patients on a regular basis (Schaffer, Sandau, & Diedrick, 2013). Despite the fact that the current healthcare opportunities allow for rather fast and efficient treatment of COPD, the readmission rates among the patients that have suffered the identified disorder remain dangerously high (Centers for Disease Control and Prevention, 2017).
It is suggested that the introduction of the strategies involving written and oral communication with patients for the further education of the latter about COPD will help reduce the levels of readmission, therefore, improving the quality of patient outcomes and promoting a rapid increase in the quality of the healthcare services.
ACE Star Change Model Overview: A Tool for Improving the Quality of Care
In order to introduce the said improvement of the healthcare environment, one will have to consider the ACE Star Model for change as the key device for compelling the nursing staff to develop the necessary skills and acquire the corresponding knowledge. By definition, the model incorporates five crucial stages, i.e., the Discovery Research, Evidence Summary, Translation to Guidelines, Practice Integration, and Outcome Evaluation (Schaffer et al., 2013).
Nurses will have to deploy the identified model since it creates the premises for the gradual development of the guidelines based on the nurses’ experience and the following text of the framework’s efficacy. As a result, the promotion of written and oral communication with patients will be assessed accordingly, and the opportunities for shaping the model to meet the needs of the target population will be created. By using the EBP-based ACE framework, one will create a pliable strategy that will give nurses enough flexibility to prevent further instances of COPD recidivism.
Define the Scope of the EBP
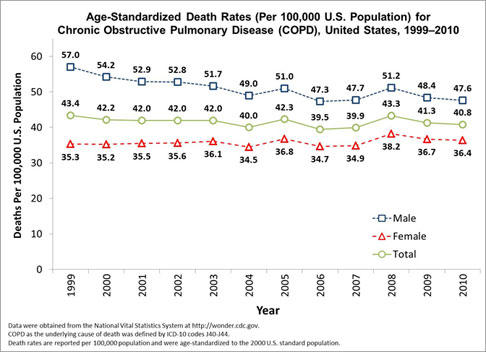
COPD readmission rates have been consistently high over the course of a few years, as shown in Figure 1. Therefore, there are solid reasons for reconsidering the current approach toward managing readmission among COPD patients. Furthermore, studies show that, on a global scale, there is currently a 20% readmission rate among COPD patients (Guerrero et al., 2016). Because of the risks to the patient’s life that readmission triggers, it needs to be managed accordingly.
Stakeholders
To make sure that the needs of the patients are met, one will have to build an interdisciplinary team. Particularly, the nurse educator, the therapist, the advanced practice nurse, and the physician will have to be viewed as the key members of the team. Helping view the problem from different perspectives, the identified experts will help design the ultimate approach toward managing readmission rates.
Determine Responsibility of Team Members
The nurse educator will play the role of promoting active knowledge and skills acquisition among patients. The therapist and the physician will determine the factors that affect the patient’s health and develop the strategy for the target population’s fast recovery. The advanced practice nurse will make sure that the required services, including the medication, are administered to the patients.
Evidence: Locating the information That Supports the Study
In the process of managing the patient’s needs, one will have to focus on gathering the relevant evidence that will inform the possible changes in the designed strategy. Apart from the clinical practice guidelines, which will be determined accordingly at the first stages of the model development, consistent acquisition of the data related to the changes in the patient’s health will have to be viewed as the key support of the study. Thus, the further choice of nursing tools will be defined.
Summarize the Evidence
Studies indicate that the promotion of patient awareness affects the quality of their outcomes to a considerable degree (Ko et al., 2016). Particularly, the use of patient education as the framework for reducing the levels of COPD readmission has proven to be a rather efficient tool for improving patient outcomes, particularly, their recovery rates, significantly (Guerrero et al., 2016). For instance, the crucial information such as the “causes, simple pathology, symptoms and treatment” (Ko et al., 2106) coupled with basic inhaling strategies has proven to have an impressively positive effect on the quality of care and the drop in morbidity rates among the target population.
Develop Recommendations for Change Based on Evidence
The existing evidence points to the necessity to enhance the communication process between a nurse and a patient. For instance, the active use of emotional intelligence (EI) as the tool for detecting a COPD-related problem at the earliest stages of its development should be viewed as a necessity. Furthermore, the focus on adopting the bedside manner approach that will allow engaging the patient in a conversation should be considered a necessity. The provision of the necessary information and skills to the target population using simple language and visuals, however, has proven to be the most important part in addressing the levels of COPD recidivism and further readmissions (Ko et al., 2016; Guerrero et al., 2016).
Translation: A Hypothetical Action Plan for Managing COPD
Action Plan
Steps
The identification of the necessary information that the patients will have to learn is the first step toward improving COPD population’s outcomes. Afterward, a series of lectures supported by visuals will have to be designed, with detailed instructions being provided to Education Nurses so that the patients could learn the essential self-management strategies.
Timeline
It is expected that the process will take four weeks. During the first week, the learning sessions will be designed. The training sessions will take place during the next two weeks. The final week will be spent on data collection and assessment of the strategy.
Assessment
The evaluation will include a comparison between the COPD admission rates before and after the intervention.
Process, Outcomes Evaluation, and Reporting
It is expected that COPD readmission rates will drop by at least 20% after the implementation of the framework. The outcomes will be measured by comparing the patient outcomes before and after the framework application. The results will be reported with the help of graphics and visuals (e.g., charts, diagrams, etc.).
Identify Next Steps
On a larger scale, the approach can be used to improve patient awareness and the quality of patient education, in general. As a result, other units will be able to use the said strategy as well. To make the implementation permanent, one will have to consider using social networks as the tools for maintaining consistent communication between a nurse and the discharged patients, as well as the community, in general.
Disseminate Findings
The local (hospital) network should be used to disseminate the study findings among the nurses. Furthermore, daily meetings with detailed reports regarding the study outcomes can be utilized. Social media, in turn, should be considered as the primary tool for data dissemination among patients and community members.
Conclusion: Improving the Outcomes in Patients with COPD
COPD is one of the disorders with the highest readmission rates. It affects the quality of patients’ lives, causing the mortality levels among the community members to rise. The focus on patient education, however, will allow managing the identified issue successfully. By using the BP strategy based on the ACE change model and deploying the principles of oral and written patient education, one will be able to improve the outcomes of the target population significantly.
References
Centers for Disease Control and Prevention. (2017). Chronic Obstructive Pulmonary Disease (COPD): Data and statistics. Web.
Guerrero, M., Crisafulli, E., Liapikou, A., Huerta, A., Gabarrus, A., Chetta, A.,… Torres, A. (2016). Readmission for acute exacerbation within 30 days of discharge is associated with a subsequent progressive increase in mortality risk in COPD patients: A long-term observational study. PLoS One, 11(3), e0150737. Web.
Ko, F. W. S., Ngai, J. C. N., Ng, S. S. S., Chan, K. P., Cheung, R., Leung, M. Y., … Hui, D. S. C. (2016). COPD care programme can reduce readmissions and in-patient bed days. Respiratory Medicine, 108(12), 1771-1778. Web.
Schaffer, M. L., Sandau, K. E., & Diedrick, L. (2013). Evidence-based practice models for organizational change: Overview and practical applications. Journal of Advanced Nursing 69(5), 1197-1209. Web.