Introduction
Health studies have often highlighted a relationship between asthma and smoking (Lee, Forey, & Coombs, 2012). Indeed, some researchers claim that most people who have asthma and smoke, at the same time are in double jeopardy because, as if tobacco smoke is not bad enough, their asthmatic condition could be triggered by irritants contained in the tobacco smoke, thereby leading to allergic inflammation of the bronchial tubes (Dutra, Williams, Gupta, Kawachi, & Okechukwu, 2014).
This condition could lead to excessive mucus production, chronic cough, and phlegm (Lee et al., 2012). For many asthmatic patients, tobacco irritants not only manifest in the aforementioned symptoms, but also make breathing difficult (Gilreath, Chaix, King, Matthews, & Flisher, 2012). The relationship between asthma and smoking explains why many adults who develop asthma past their 50th birthdays often have a history of smoking tobacco (Dutra et al., 2014). My topic of study is centered on exploring the relationship between asthma and smoking among adult African Immigrants in California.
This study is important because African immigrants are a relatively understudied group. Furthermore, they are mostly underinsured than the general American population and experience significant variations, in terms of education and income outcomes, relative to other ethnic groups as well (Dutra et al., 2014). Because of their low socioeconomic status, they often experience inadequate medical care, which is often characterized by a lack of access to health care (Dutra et al., 2014; Gilreath et al., 2012).
This problem often creates an inadequate recognition of asthma severity and the under-prescription of controlled medications by health care service providers. Besides poor socioeconomic conditions, African immigrants also suffer from other risk factors such as environmental exposures (because of the difficult working conditions they are often subject to) and respiratory tract infections that are often associated with low-income living (Dutra et al., 2014).
This study would have a positive impact on social change because it could help to reduce the impact of asthma incidences within the target population. Such an outcome would come, in part, from understanding the relationship between smoking and asthma. Understanding the relationship between the two variables could also help to improve the health outcomes and wellbeing of immigrant populations in California.
The process could also shed more light on the factors that affect the relationship between the same. The insights drawn from this study could also be instrumental in understanding the social, economic, and political factors associated with Africans as an immigrant population in California. This analysis would provide a better understanding of their health outcomes and overall wellbeing. Additionally, the findings of the study would help to expand the body of research explaining the relationship between asthma and smoking among African immigrants in California, and, by extension, immigrants. Thus, this study could promote positive social change by informing health policy decisions regarding smoking and asthma management in the state of California.
This first section of the study starts with a background review of the research topic and focusing on the research gap. That is followed by the problem statement, the purpose of the study, the research question, and the research hypothesis. I will then present the theoretical framework which this study is grounded on. The next topic will be the approach or nature of the study. The literature review starts with the literature search strategy followed by an extensive review of literature related to key variables and concepts. Key definitions, study assumptions, scope and delimitations, and limitations of the study will then be presented. The final part of this section will be to explain the significance of this study followed by a brief summary and conclusion.
Problem Statement
Researchers and medical experts have investigated the relationship between asthma and cigarette smoking. This relationship is founded on the fact that cigarette smoking causes the settlement of irritating factors on the air pathways, thereby worsening asthma attacks, or causing their resurgence (Tamimi, Serdarevic, & Hanania, 2012). Similarly, smoking often damages small hair-like structures (cilia) on the air pathways rendering them ineffective, thereby triggering asthma attacks (Tamimi et al., 2012). According to Currie and Baker (2012), about 25% of asthma victims are cigarette smokers.
African and Hispanic immigrants suffer a high risk of asthma fatalities compared to major ethnic groups in California (Findley & Matos, 2015). This is large because of socioeconomic disadvantages, poor housing conditions, and the lack of proper access to health care services (Findley & Matos, 2015). Smoking is also a contributor to this outcome because different studies have shown that many African immigrants often continue their smoking habits after arriving in the US (Amer & Awad, 2015). Researchers that have further investigated this issue point out that, West African immigrants experience fewer inhibitions to smoking because of a group-based cultural identity theory, which presupposes that they are free to smoke in America because of fewer social inhibitions that often prevented them from doing so in their home countries (Gatrell & Elliott, 2014). Nonetheless, this habit contributes to their poor health outcome.
Another set of contributors to the poor health outcome among African immigrants is the nature of jobs that they do in America. As shown by Braback, Vogt, and Hjern (2011), most immigrants often work in low-paying jobs that expose them to indoor and outdoor air pollution, which affects their overall health. Most of these jobs are concentrated in the agricultural, construction, and service sectors (Gatrell & Elliott, 2014).
Some of the materials used in these industries contain harmful chemicals that further jeopardize their general health. For example, glues, insulation, and wood products contain harmful chemicals that are known to negatively influence the health of people exposed to them (Braback et al., 2011). Paints, cleaning products, and carpets also contain similar harmful chemicals, such as formaldehyde, which cause respiratory health complications.
Researchers have investigated the relationship between asthma and smoking among different races and different genders. Corlin, Woodin, Thanikachalam, Lowe, and Brugge, (2014) assessed the relationship between asthma among Chinese immigrants living in Canada and their smoking behaviors. Other researchers have also investigated this relationship, relative to patients’ country of origin, area of residence, and education studies. Gatrell and Elliott (2014) explored the relationship between geographic differences and health status among immigrant groups in the US.
Most of the studies are based in developed countries that do not have many immigrant groups, and some of the studies are outdated. Few of these studies reflect the continuing changes in immigrant status or explain the relationship between smoking behaviors and asthma cases in regions that have multiple immigrant population groups, such as New York and California.
Although there are African immigrants residing in the US, many health studies have often categorized them as African-Americans, thereby failing to draw the distinction between the health outcomes African-Americans and African born US residents (Schenker, Casta-eda, & Rodriguez-Lainz, 2014). Furthermore, this population group is one of the understudied in the area of immigrant health because researchers have mostly focused on studying Hispanics and Asian immigrants. Citation The neglect of African immigrants, as a significant health cohort worth studying, betrays the spirit of public health, which promotes the provision of a holistic picture of health management (Moreland-Russell & Brownson, 2016). With this proposed study, I seek to fill this research gap by exploring the association between asthma and smoking among adult African immigrants in California.
Purpose of the Study
The purpose of this study is to determine the association between asthma and smoking status among adult African immigrants residing in California. I intend to use a quantitative correlational approach to explore the association between asthma and smoking status and selected demographic variables among adult African immigrants in California. The independent variables will be smoking status, age, sex, years since immigration, marital status, alcohol use, education level, income level, and employment status, and the dependent variable will be asthma.
As highlighted in this paper, this study is a secondary analysis of archived data relating to the incidence of smoking and asthma among immigrant groups (Africans) in California. The data are presented in the California Health Interview Survey, which is an annual health database in the state. The data were developed from a telephone interview of more than 20,000 Californians and is considered the largest in America (Elk & Landrine, 2012).
The CHIS database is appropriate for this study because it is not only free but also authoritative and easy to use. I also chose to use this database as the main source of data for this study because it is credible and reliable. In fact, different professionals have used it to conduct health needs assessments, health research, and grant proposals (Elk & Landrine, 2012). Others have used it in news reporting and policy-making with great success. This record of accomplishment affirms its reliability.
Research Question and Hypotheses
The quantitative research question, hypotheses, and research variables for the proposed study are stated below:
- RQ–: What is the association between asthma and smoking status among adult African immigrants in California?
- Null Hypotheses (H0): There is no association between asthma and smoking status among adult African immigrants in California.
- Alternative Hypothesis (H1): There is an association between asthma and smoking status among adult African immigrants in California.
- Dependent Variable (DV): Asthma.
- Independent Variable (IV): Smoking status.
- Mediating Factors: Age, sex, years since immigration, marital status, alcohol use, education level, income level, and employment status.
- Study Group: Adult African immigrants in California.
Theoretical/Conceptual Framework
The socio-ecological theory will be the main conceptual framework for this study. Introduced in the 1970s by sociologists coming from the Chicago School, and revised by Bronfenbrenner throughout the 1970s and 1980s, this theory has been used to merge behavioral issues and anthropology issues in health studies (Moore, de Silva-Sanigorski, & Moore, 2013). The theory has five nested levels of interlocking behavioral and anthropological factors – interpersonal, organization, community, individual, and policy enabling environments. The interaction of these levels is summarized in the diagram that follows:
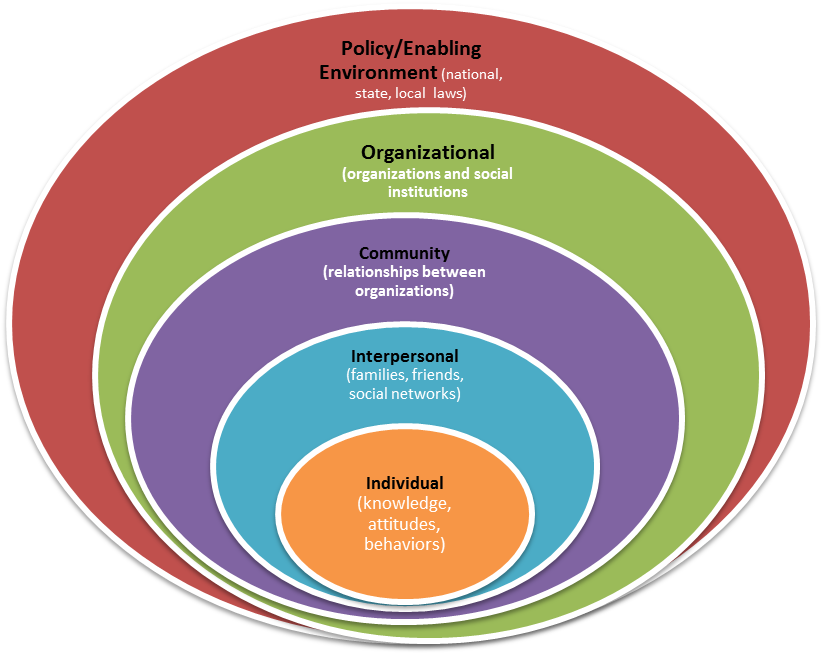
A key contribution of this theory to different fields of health and psychology is the understanding that the true comprehension of human growth should occur through a complete understanding of the ecological system, which supports or influences their behaviors (Yakob & Ncama, 2016).
The rationale for using this theoretical framework in this study stems from its ability to show different levels of personal and environmental factors affecting human behaviors and health outcomes. It does so by considering the complex interplay between the five layers of personal and environmental factors mentioned. This also justifies its application in this study because it has been used to successfully prevent domestic violence, child abuse, and promote community health (among other contributions in public health) (Gilioli, Caroli, Tikubet, Herren, & Baumgärtner, 2014). Its success in community health promotion is the main motivator for applying the theory in this study.
The socio-ecological model is ideal because it provides a holistic understanding of my research topic. Moreover, it takes into account the environmental factors that could affect the relationship between asthma and smoking (Sharma, 2016). The multifaceted nature of the model is appropriate for the study because I will explore the impact of several mediating factors, such as education, work, age, sex, and income (among other factors) in exploring the association between asthma and smoking among adult African immigrants in California (Coutts, 2016). In this regard, the model aligns with the variables of the study.
The socio-ecological model also incorporates our understanding of sociocultural factors that affect smoking behaviors among African immigrants because, as shown by previous studies, the smoking habits of this group of immigrants is partly caused by cultural factors (Bosdriesz et al., 2013). The socio-ecological model would help me to understand this bit of the analysis as well. Lastly, this model fits with the significance of the study, which is to inform public health policies and strategies regarding asthma management because the theory can provide a framework for preventing health problems.
This theoretical framework is relevant to my research issue because it would help me to uncover the personal and environmental factors that could explain an association between asthma and smoking among African immigrants (Onono et al., 2015). Marshall (2016) says smoking is a personal issue that is often associated with environmental factors, such as culture, peer influence, stress, and such factors. Similarly, asthma is a personal and environmental issue because it could be triggered or exacerbated by biological or environmental factors. Immigration also changes the environmental context that could affect human health outcomes (Arsen, 2013).
In this regard, this framework could help to explain the environmental issues of African immigrants in California that could affect their health status. This way, this theory is useful to my research study because it provides a holistic perspective of our research issue. More specifically, it incorporates all my research variables because smoking is a sociological (behavioral) issue, while the health issue (asthma) affecting African immigrants living in California could be moderated by environmental factors.
Nature of the Study
I will use the quantitative correlational approach in the proposed study. This quantitative correlational approach aligns with the primary research question, investigating if there is an association between asthma and smoking among adult African immigrants in California. The asthma status is a quantitative measure because data on asthma reporting is usually presented in numbers. Similarly, smoking is often measured in terms of the number of people who do it. These two sets of data for the research variables are quantitative in nature. Therefore, the selection of the quantitative technique is a natural process, based on the nature and characteristics of the variables that are measured (Creswell, 2014).
The quantitative approach is applicable to this research because my main source of research information – the California Health Interview Survey (CHIS) dataset and codebook is quantitative in nature. There are different types of research approaches in quantitative studies. The main ones include descriptive research, correlation research, quasi-experimental research, and experimental research (Jacobsen, 2016).
The correlation approach is the main approach to this study because it focuses on determining the existence and extent of a relationship between two or more variables. It aligns with my research topic because I also strive to investigate the association between asthma and smoking among adult African immigrants in California. Thus, the justification for using the correlation approach rests in the fact that it seeks to find out and interpret relationships between different variables (Guest, 2014).
The California Health Interview Survey (CHIS) is a statewide survey that contains quantitative data about different health issues in California. Supported by the California Department of Public Health and the Department of Health Care Services, this database contains health data obtained from telephone surveys that include the views of thousands of California residents (UCLA Center for Health Policy Research, 2017).
As highlighted in this paper, my research topic is centered on investigating the association between asthma and smoking among adult African immigrants in California. The research variables for this study include asthma, as the dependent variable, smoking as the independent variable, and age, sex, years since immigration, marital status, alcohol use, education level, income level, and employment status as mediating variables, or covariates.
Literature review
Literature Search Strategy
I conducted the literature review using reputable sources of peer-reviewed articles available from Google Scholar, Google Books, NCBI, and MEDLINE. Most of the articles sourced from these databases are openly available. The key research terms used to get the articles were “African,” “Immigrants,” “Asthma,” and “Smoking.” Most of these terms were derived from the variables under study and the nature of the research topic. All the sources consulted in this review are not more than five years old (they are published between 2012 and 2017). Excluded from the review were research articles that were published earlier than in 2012. I also excluded articles that came from commercial websites, blogs, and other online sources that were unreliable.
Literature Review Related to Key Variables and Concepts
Prevalence and Incidence of Asthma
The prevalence and incidence of asthma worldwide vary across different regions and countries. According to the American Academy of Allergy, Asthma, and Immunology (2017), about 300 million people suffer from the condition globally. Similarly, there are 250,000 annual deaths attributed to the same condition, globally (American Academy of Allergy, Asthma, and Immunology, 2017). The number of people suffering from the condition is expected to increase dramatically by more than 100 million (American Academy of Allergy, Asthma, and Immunology, 2017). Thus, experts estimate that in 2025, the global population of people who will be suffering from asthma would be 400 million (Naturopath, 2013). Researchers claim that poor workplace conditions, such as exposure to toxic fumes, are responsible for the increase in asthma incidences (Naturopath, 2013).
In the US, it is estimated that one in 12 people suffer from the condition (Naturopath, 2013). This figure is equivalent to 25 million people and it represents 8% of the country’s population. Reports show that 53% of the American population, which suffers from asthma, had suffered an attack as well (Naturopath, 2013). However, this number is skewed towards children because there are more asthma attacks among children than in adults. However, statistics from 2008 to 2010 show that the incidence of asthma is higher among minority racial and ethnic groups in America, compared to the white population (Naturopath, 2013).
In California, it is estimated that more than 5 million adults suffer from asthma (CDC, 2014). Health agencies also point out that more than 1.7 million children suffer from the condition in the state (CDC, 2014). The state reports more than 500 deaths associated with this condition. The CDC (2014) adds that 145,000 annual emergency room visits in California are associated with this condition. Based on these statistics, asthma is not only a significant health problem in California but also a national problem for America and a global health issue for many countries.
Prevalence and Incidence of Smoking
According to the World Health Organization (2016), more than 1 billion people smoke tobacco worldwide. Statistics show that more men than women make up this number of smokers (World Health Organization, 2016). Similarly, they show that although the incidence of smoking is declining globally, the Mediterranean and African regions are still recording an increase in the incidence of smoking (World Health Organization, 2016).
This finding means that smoking is primarily a problem that is concentrated among developing countries and within lower socioeconomic groups. Indeed, out of 5 million deaths that occur globally because of smoking, more than two-thirds of them are concentrated in developing countries (World Health Organization, 2016). These deaths are projected to increase because the number of smokers is expected to grow to between 1.5 billion – 1.9 billion in 2025 (World Health Organization, 2016).
In the US, cigarette smoking is attributed to be the leading cause of preventable diseases (CDC, 2015). Statistics show that it accounts for more than 480,000 deaths annually (CDC, 2015). Additionally, the CDC (2015) says there are about 15 smokers out of a population of 100 Americans. This figure translates to 15% of the population being smokers. Generally, there is a decline in the incidence of smoking in America because the above figure represents statistics reported in 2015. In 2005, the figure was 21% (CDC, 2015). Nonetheless, based on the current incidence of smoking, the CDC (2015) says that 16 million American smokers live with a smoking-related disease.
The prevalence of smoking in California follows a decline in the number of smokers nationally. However, researchers estimate that the state has a tobacco smoking prevalence of 11% (Walters, 2015). This is below the Healthy 2020 goal of 12%; meaning that California is among the few states that have met its Healthy 2020 goal of reducing the smoking prevalence to less than 12%. Statistics show that black Californians have the highest prevalence rate of smoking in the state (Walters, 2015). The incidence of smoking is also more prevalent among low-income populations than in other socioeconomic groups. These findings show that smoking is a state, national, and global health problem.
Conceptual Framework
The socio-ecological model will be the main conceptual framework for this study. However, other researchers have used other types of conceptual frameworks to explore the interaction between human factors and environmental factors while trying to assess or predict health outcomes. Kapp, Simoes, DeBiasi, and Kravet (2016) used the systems theory to investigate how immigration patterns affect health outcomes in America.
Jayasinghe (2015) also used the same conceptual framework to explain how social issues affect health outcomes. Both researchers said that the systems theory provided a reliable conceptual framework for understanding how natural and social systems interact. They also said that the same framework properly conceptualized population health outcomes as dynamic, open, and adaptive systems. Broadly, these researchers have managed to demonstrate that human health outcomes are products of interrelated parts of subsystems, thereby enhancing our understanding of interactions between micro-meso-macro levels of health (Jayasinghe, 2015).
Researchers have also used the social construction theory as another conceptual framework for understanding the interrelations between different health variables. As highlighted in the works of researchers such as Onono et al. (2015), this theoretical foundation explains how socio-cultural and historical factors often shape people’s health outcomes. This theory would have been relevant to our research issue because it has been used by many researchers to explain the lived experiences of oppressed or minority communities. However, the main flaw of this theory (regarding its use in our research study) is its excessive bias on cultural and historical factors as a predictor of health outcomes. In this regard, it has no proper consideration of other factors that could affect health outcomes.
The main issue to point out in this analysis is that these conceptual frameworks have mostly been used to effect change or institute human behavioral changes as a prerequisite for their use. This focus does not explain the nature of this study because it does not institute change. Instead, it merely strives to describe a health phenomenon. The socio-ecological model adopts a broader view of health issues. This is why it was the most appropriate model for quantitative research.
Effects of Immigration on Health
Different researchers have explored the relationship between immigration and asthma. Such is the case of Cabieses, Uphoff, Pinart, Antó, and Wright (2014) who conducted a systematic review to analyze the effect of immigration on the relationship between asthma and smoking. They conducted this review according to the guidelines stipulated in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) and found that there were significant differences in allergic reactions for populations that lived in their countries of origin and those that emigrated to other countries (Cabieses et al., 2014).
They also found that the level of development in the host countries significantly affected the level of asthma developed by the immigrants. Fox, Entringer, Buss, DeHaene, and Wadhwa (2015) have also demonstrated that immigrants who lived in developed countries had higher rates of asthma compared to those who lived in less developed countries. The researchers also established that there was a strong influence of the environment on the development of asthmatic conditions among the sample populations (Fox et al., 2015). Additionally, they established a higher prevalence of asthma among second-generation immigrants compared to first-generation immigrants because the latter group was not exposed to the environmental conditions of the host countries as much as the former group.
This assertion showed that the length of stay in the host country was directly related to the development or seriousness of asthmatic conditions. These findings were consistent with research studies conducted by Ro (2014), which upheld the same conclusion across sample groups of different nationalities, study populations, and age groups. However, he established differences across these social groups when the linear model was used (Ro, 2014). The differences also emerged when the respondents compared the findings across the early and later stages of immigration. Differences in time of residence also yielded the same outcomes.
In a different study to investigate asthma incidences among Asian immigrants living in America, Becerra, Scroggins, and Becerra (2014) established that Chinese, Filipino, South Asian, and Japanese immigrants reported a positive relationship between asthma and immigration. The same was true for Korean immigrants because the study showed that there was a positive relationship between asthma prevalence and immigration status (Becerra et al., 2014). The researchers used a linear regression model to come up with the findings after relying on data prepared by the California Health Interview Survey 2001-2011.
Garcia-Marcos et al. (2014) also conducted a study to investigate whether immigration affects asthma incidences among immigrants and came up with the same findings. In other words, they established that immigrants to western countries often adopt the same allergic reactions that host populations suffer from. The researchers used a mixed-method approach to conduct the review by first gathering data using questionnaires from 13-14-year-old immigrants living in the USA. They also gathered the views of parents who had children aged 6-7 years old using secondary research data (Garcia-Marcos et al., 2014).
Their findings showed a weak association between immigration and higher incidences of asthma. Thus, they believed that the reduced risk of asthma was often related to immigrants who had lived in America for the shortest time. This finding is consistent with the views of Lopez and Golden (2014) who say an increased stay in the host countries, often leads to the loss of a protective pre-immigration environment that would have otherwise helped immigrants to lower their risk of asthma.
Corlin, Woodin, Thanikachalam, Lowe, and Brugge (2014) investigated how immigration affected the health outcomes of Chinese immigrants and after sampling the health outcomes of more than 147 immigrants, they established that the immigrant population had better health outcomes compared to the native populations. The researchers also used bivariate and multivariate models to compare the prevalence of diseases among the two population groups, as well as the clinical biomarkers associated with the study focus (Corlin et al., 2014). To explain their findings, the researchers said that healthier diets, minimal exposure to cigarette smoke, and increased physical activity among the Chinese immigrants were mostly responsible for their positive health outcomes.
Also, Corlin and Brugge (2014) conducted an independent research study to investigate the incidence of asthma among immigrant populations and found that there is a “silent epidemic” of asthma among immigrant subpopulations in America. The authors said the epidemic was largely unreported because of poor access to health care services within this immigrant population.
Camacho-Rivera, Kawachi, and Bennett (2015) also investigated the relationship between immigration and health outcomes by exploring the effect of race, ethnicity, and country of origin on the risk of developing asthma. The researchers used 2,558 non-Hispanic white and Hispanic children to investigate this research phenomenon and found that lifetime asthma incidence was prevalent in less than 9.1% of the population (Camacho-Rivera et al., 2015). They also found no significant differences in asthma rates between Hispanic and non-Hispanic respondents. This study highlighted the importance of moving beyond racial or ethnic classifications to develop policies surrounding asthma management because these classifications often mask different subgroups of people who are at high risk of asthma.
Barr et al. (2016) conducted a study to test whether ethnicity is a dependent variable in the prediction of asthma incidences among immigrant populations in the US by analyzing whether the condition was prevalent among Hispanics and Puerto Ricans more than other immigrant groups. They found that asthma was more prevalent among second-generation Hispanic and Puerto Rican immigrants than first-generation immigrants were (Barr et al., 2016). They partly explained this finding using differences in smoking patterns among the sampled population groups. Their study included a sample of 16,415 Hispanics and Latinos (Barr et al., 2016).
In a different study to evaluate asthma admissions using ethnic variations, Sheikh et al. (2016) found that South Asian immigrants reported the highest hospital admissions attributed to asthma. These findings were developed after evaluating two main ethnic groups – whites and South Asian immigrants. However, the researchers failed to take into account sex-related differences that would have affected health outcomes.
Benchimol et al. (2015) also used South Asian immigrants as a sample group to estimate the incidence of asthma and immune-mediated diseases among immigrants in western countries. They used population-based cohorts of respondents who suffered from asthma and diabetes to undertake the review and found that adults from South Asia had a higher predisposition to asthma compared to other ethnic immigrant groups (Benchimol et al., 2015). This finding contradicted the view of many studies highlighted in this literature review because other studies have consistently shown that immigrants from other countries had a lower risk of developing asthma compared to host populations. However, the explanation for this inconsistency could stem from the fact that the findings of Benchimol et al. (2015) are mostly attributed to a genetic predisposition to the disease among South Asian immigrants.
Mahmoudi (2016) conducted a broader review involving more than 40 countries to understand the effect of immigration on asthma incidences and found that immigration was associated with a low incidence of asthma. He developed these findings after conducting a survey of more than 326,000 adolescents from more than 40 countries. The survey also included a population of 207,000 children from 30 countries (Mahmoudi, 2016). However, the association between immigration and asthma incidence was limited to affluent countries. The findings of Hamilton, Cardoso, Hummer, and Padilla (2011) would be useful to our proposed study because they would explain how immigration affects the health outcomes of immigrants in California. Their findings stem from a review of how assimilation has affected the health outcomes of immigrant children in America.
Reed and Barosa (2016) have also explored the role of the nativity in explaining the advantage enjoyed by immigrants compared to their host populations when it comes to asthma prevalence. To explain this advantage, they explored the health outcomes of two groups of immigrants – refugees and non-refugees. The findings revealed that refugees were disadvantaged when it came to accessing health care services, thereby suffering poor health outcomes compared to their non-refugee counterparts. Comprehensively, these studies show there is an association between asthma and immigration, with immigrants suffering lower incidences of asthma compared to host populations.
Effect of Environmental Exposures on Health
In an effort to understand the effects of environmental exposures on health, Im et al. (2015) outlined the case of a researcher, Johnson, who used an innovative framework to separate a host of factors affecting asthma incidences into different constituents. His analysis concentrated on factors that affect the design, construction, and conditions of the dwellings, which immigrants lived in. The researcher found that the risk of developing asthma was directly correlated to the nature and type of dwelling (Im et al., 2015). Im et al. (2015) said this relationship was a product of the interaction between culture and environment.
In a separate study, Rumrich and Hänninen (2015) found that the complexity associated with asthma management was directly associated with the immigrants’ ability to communicate fluently in English and partly on whether they were born in the U.S, or not. They also established that asthma was more severe for immigrants who were relatively acculturated to their host countries, compared to those who were not (Rumrich & Hänninen, 2015).
Their findings correspond with a similar study by Chiu et al. (2016), which highlighted the lower incidence of asthma among new immigrants compared to those who had been in the host nations for a long time. This comparison implies that western risk factors increased the risk of developing asthma. This fact was supported by studies, which investigated the same issue among Arab-Americans (Im et al., 2015).
Rottem, Geller-Bernstein, and Shoenfeld (2015) established that environmental factors and the age of immigration affected people’s predisposition to asthma. The researchers went further to explain that the level of immunoglobin E was relatively higher among immigrants compared to the local population, thereby decreasing their predisposition to asthma (Rottem et al. 2015). The researchers also explored the possibility of a reversal of allergies because of parasitic infections. In this regard, they proposed that secondary prevention guidelines should be introduced to immigrants before they settle in their host nations, as a strategy to prevent asthma attacks (Rottem et al. 2015).
Gatrell and Elliott (2014) also conducted a similar study by exploring the relationship between geographical location and health status among immigrants. Although the study assessed different health variables, it found that geographical differences significantly affected the incidences of asthma among immigrants.
Studies that have tried to explore the impact of the environment on the health of immigrants have found it difficult to isolate the environment from other socioeconomic factors affecting immigrants that would ultimately affect their health as well (Okechukwu, Souza, & Davis, 2014). For example, a study by Guruge, Birpreet, and Samuels-Dennis (2015) to investigate the impact of environmental conditions on older women immigrants in Canada found that SES, cultural beliefs, gender norms, and influences of the physical and social environment weighed heavily on immigrant health. The studies also showed that older immigrant women were more likely to have health problems because of poor access to health care services and the underutilization of preventive health services (Guruge et al., 2015).
Martinez et al. (2015) contend that some of the problems faced by immigrants living in America are partly caused by unfavorable immigration policies. For example, they say unfavorable immigration policies often affect access to health care issues (Martinez et al., 2015). They arrived at these conclusions after reviewing eight health databases, which showed that anti-immigrant sentiments often affected the health outcomes of immigrants because it limited their ability to access health care services. Rhodes et al. (2015) have also come up with similar findings after investigating the effect of immigration policies on immigrant health in America.
Flynn, Carreón, Eggerth, and Johnson (2014) say that understanding the impact of someone’s work environment on their health goes beyond merely understanding how their work presents social hazards and risks to their wellbeing. Indeed, as explained by Arcury (2014), someone’s work also affects other aspects of their social wellbeing, and by extension, their health (work is the major incentive for many people who emigrate to the U.S).
According to Pichardo-Geisinger et al. (2014), many immigrant groups often experience deteriorating physical health after working in the US for some time. They made this finding after reviewing the physical health of a group of Latino immigrants working in the US. The link between work and immigration occurs through the understanding that work often alters the physical environment of immigrants, thereby putting their physical health and those of their family members at risk of deterioration.
Shani et al. (2013) explored the relationship between Asthma among Ethiopian born immigrants and of those living in western countries. They found that the intensity of asthma increased after their travel to western countries. The researchers used 1,217 matched controls for a population sample of the same number of immigrants and found that asthma incidences among second-generation immigrants did not significantly differ from those of the native population. The findings affirm the view that environmental exposures affected asthma incidences.
Socioeconomic Status and Asthma
The effect of socioeconomic status (SES) and asthma have emerged in several research studies that have tried to investigate the relationship between immigration and asthma incidences. Most of these studies have developed findings that have overlapped with similar findings from researchers who have studied the influence of the environment on the incidence of asthma attacks. According to Acton (2012), most immigrant groups living in America have a lower socioeconomic status. In fact, he says that most of them have household incomes that are below $50,000 (Acton, 2012). Most of the houses or dwellings that these immigrants live in are overcrowded.
Kelly, Glick, Kulbok, Clayton, and Rovnyak (2012) estimate that one-quarter of them are this way. Owing to these conditions, most of these homes create adverse environmental conditions, such as dampness or molds (44%), pests (28%), and poor ventilation (26%) (Acton, 2012). These conditions are known to increase the incidence of asthma and atopic diseases. Similar studies have shown that at least one of the aforementioned adverse conditions was found in at least 67% of homes inhabited by immigrants (Kelly et al., 2012). Furthermore, they found that multiple hazards were present in more than 27% of similar homes inhabited by immigrants. Grzywacz et al. (2012) say that children of recent immigrants showed symptoms of asthma one year after immigration. In detail, these symptoms were suggestive of asthma (4%) and atopic disorders (10%). Nonetheless, they often suffered from poor diagnosis because only 2% of this population was diagnosed with asthma or atopic disorders.
Reingle, Caetano, Mills, and Vaeth (2014) demonstrate that although the incidence of asthma among Mexican immigrants was lower than other immigrant groups, it was mostly attributed to poor housing conditions. A scholar, J. S. Slitt, and his colleagues from the University of Colorado said that the most common housing issues affecting this immigrant population were plumbing leaks, development of mold, dampness, and pest infestation (Sternberg et al., 2016). Based on these findings, the researchers proposed that asthma management strategies should be multifaceted and more importantly address housing issues and access to health care concerns.
Studies conducted by Landsbergis, Grzywacz, and LaMontagne (2014) have also shown that lower SES is often related to increased asthma incidences, especially among immigrant populations. Differences in race and ethnicity have also been associated with higher rates of asthma attacks, as explained by Abraído-Lanza, Echeverría, and Flórez (2016) who say that the two factors are predictors of health indicators, such as access to health care and health insurance. The disproportionate nature of asthma and SES has led many researchers to delineate this relationship and to highlight the underlying factors that moderate this relationship.
For example, Borges, Orozco, Rafful, Miller, and Breslau (2012) conducted a study to investigate the extent that SES influences asthma incidences among African-American immigrants and Latino youth. Studies that have undertaken the same analysis have used parental SES, education standards, and family income as predictors of SES (Kelly et al., 2012). Their findings have generally shown that decreasing SES scores were directly associated with increased adjusted odds of asthma. Nonetheless, as explained by Riosmena, Wong, and Palloni (2013) these studies have also shown that acculturation was among the strongest moderating variables for understanding the incidence of asthma among immigrant populations.
Studies that have investigated the impact of SES on asthma incidences have also studied African-American populations in America and found that the poorest children were most affected by asthma (Carroll, 2013). The same finding was revealed in studies that investigated the same research issue among non-Hispanic blacks and non-Hispanic white populations (Kelly et al., 2012). In ethnic-stratified models, researchers such as Thakur et al. (2013) and Beck, Simmons, Huang, and Kahn (2012) have not found statistically significant relationships between maternal education levels and asthma incidences across different ethnic or racial groups.
However, in small high-risk cohorts of children within the Hispanic communities, there was a relationship between ethnicity and asthma levels when the researchers adjusted different SES metrics. One advantage of these studies is the requirement that the respondents identify themselves as African-American or Hispanic before being included in the study (Thakur et al., 2013). This provision helped the researchers to capture the cultural influences that would have affected their research outcomes. In addition, the respondents included in the study must have had a physician diagnose them as asthmatic within the past two years. There was also a control population, which included respondents without any symptoms of asthma or any prior diagnosis of the same condition (Beck et al., 2012).
Considering the collective research one can conclude that SES could affect the incidence of asthma among different racial and ethnic populations in the US. This fact outlines the presence of different confounding factors that could ultimately affect the relationship between SES and asthma incidence. Generally, these studies have shown that urban populations living in low-income settlements suffer a high risk of asthma because they are exposed to harmful indoor allergens that increase their predisposition to asthmatic attacks.
Outdoor pollutants have also been established to exacerbate their asthmatic conditions (for those who suffer from the condition in the first place). Relative to this fact, Carroll (2013) adds that “child psychosocial, socio-emotional, and anthropometric factors, such as obesity, are associated with both low SES and asthma, and thus are important exposures to consider when attempting to delineate the relationship between SES and asthma, and potential effect modification by race/ethnicity” (p. 1180).
Gong et al. (2014) emphasized the need to understand the effect of social and economic influences on asthma incidences after evaluating how parental SES affects the risk of asthma among their offspring. The researchers established that there was a direct relationship between household income levels and the health outcomes of children growing up in the same settings (Gong et al., 2014). The researchers also established a relationship between asthma incidences and educational levels within different household settings because there was an association between high education levels and lower risks of asthma, as well as an association between high incidences of asthma and lower education levels. They developed these findings after studying a cohort of 211,500 children born between 2006 and 2008 (Gong et al., 2014).
Keet et al. (2015) investigated whether neighborhood poverty and residence status (inner city and non-inner cities) were associated with asthma incidences. Their study aimed to evaluate whether residency status within inner cities and non-inner cities could help to predict the incidence of asthma (Keet et al., 2015). After conducting a secondary analysis through a national database, the researchers found that inner-city residency was associated with higher incidences of asthma (Keet et al., 2015).
However, this association was not statistically significant after adjusting for specific social variables, such as race, ethnicity, and religion. Based on these findings, the researchers claimed that although the incidence of asthma was highest among inner-city neighborhoods and among specific immigrant populations, such as Hispanics and Puerto Ricans, demographic factors mostly explained this relationship, as opposed to inner-city residency (Keet et al., 2015). This finding contradicted the views of some researchers highlighted in this paper who said SES could be used to assess the risk of developing asthma. Instead, it draws our attention to demographic factors, as opposed to SES, as a predictor of asthma incidences.
Celedón (2016) investigated health inequality between immigrants and US-born citizens and found out that there are significant health disparities between the two groups. Her findings would be instrumental in our proposed study because they would help us understand the impact of socioeconomic factors on health outcomes among immigrant groups. In another book titled, “The Immigrant Health,” Loue (2013), shows the flip side of immigrant health by saying socioeconomic factors have always made it difficult for immigrant populations to gain access to health care services, thereby increasing their incidence of asthma. Streja et al. (2014) also contributed to this discussion by saying poor living conditions have increased secondary smoke exposure to children born in immigrant families, thereby increasing their incidence of asthma. Passive smoking is an issue with regards to Asthma attacks.
Effects of Smoking on Health
Many studies have investigated the relationship between smoking and asthma. Different immigrant groups in America report different levels of smoking. In one study conducted by Burgess (2014), South East Asian communities living in America are among the heaviest smokers. After collecting the views of 60 leaders within this ethnic group (using semi-structured interviews), the researchers also discovered that smoking tobacco was a cultural heritage issue for this immigrant group (Burgess, 2014). In other words, it was used to convey social status and was a symbol of respect.
Furthermore, the study revealed that many older social males suffered from isolation and smoked to alleviate the stress associated with it (Burgess, 2014). Based on these assertions, the findings suggested that community leaders in South Asian immigrant communities needed to promote a cultural shift in smoking to prevent their members from promoting this habit.
Allem et al. (2012) conducted a study to investigate how the environment often affects smoking habits when immigrants move from their countries of origin to America. After investigating the smoking behaviors of Koreans in Seoul and Koreans in America and collecting data using telephone surveys, they found that smoking patterns differed for both groups of Koreans (Allem et al., 2012). Although they found that there was a peak in the relationship between smoking habits and immigrants’ age, at 35 years, they found that South Koreans living in America smoked more than those living in their home countries (Allem et al., 2012). They mostly attributed this finding to social role transitions between Koreans living in America and those living in their countries of origin.
In a study to investigate the smoking-related mortality rates among Latino and Hispanic immigrants, Fenelon (2013) found that these immigrant groups had lower levels of smoking-related deaths compared to whites living in America. This finding was established, irrespective of the low SES of the immigrants (Fenelon, 2013). However, culture was established as a moderating variable that could influence the smoking patterns between immigrants and populations living in the host nations.
Bosdriesz et al. (2013) explored the prevalence of smoking behaviors among immigrant groups by comparing such trends to smoking behaviors in their host countries and with the general US population. They found that the prevalence of smoking behaviors among immigrant groups was lower than the prevalence of smoking among the US population. These findings will be instrumental in our proposed study because they would help us to understand smoking behaviors among various immigrant groups.
Cho and Paik (2016) conducted a different study to investigate the same research health issue (asthma) but assessed it by investigating the relationship between e-cigarettes among South Korean immigrants, as the chosen study population. After assessing a sample of 35,904 students, the researchers pointed out that there is a positive relationship between e-cigarette consumption and increased asthma incidences.
Generally, these findings have shown that smoking worsens people’s health. The evidence supporting this assertion is abundant. For example, in one study conducted by Polosa, Caponnetto, and Sands (2012) to care for smoking asthmatic patients, it was established that smoking asthmatic patients could present a distinct disease entity, which manifests as asthma complications and chronic pulmonary disease obstructions. In the assessment of asthma management, smoking could have clinical and prognostic implications. Nonetheless, the researchers pointed out that smoking severely increases the impact of asthma attacks (Polosa et al., 2012).
Spears et al. (2013) also arrived at the same conclusion when he investigated the incidence of asthma among affected persons who started smoking. To meet his objectives, the researchers conducted an exploratory study on three groups of respondents. The first one comprised of 22 current smokers. The second one was made up of 21 people who had never smoked. The last group comprised of 10 ex-smokers. The researchers examined their blood and sputum cytokine concentrations to understand the effect of smoking on their risk of asthma. The results showed that smoking had increased sputum cytokine levels, thereby supporting the view that smoking increased the risk of asthma (Spears et al., 2013).
Role of Acculturation
Researchers, such as Reiss, Razum, and Lehnhardt (2015) have explored the impact of acculturation on the smoking habits of different immigration groups and found gender differences in immigration smoking patterns between men and women. Men reported the highest smoking incidence compared to women. Similarly, women who had undergone years of acculturation were more susceptible to smoking compared to those who had not (Reiss et al., 2015). The researchers came up with these findings after retrieving and analyzing 27 studies published between 1998 and 2013. Generally, they pointed out that, different groups of immigrants from different countries had reached different stages of smoking where non-western countries were in the early stages of smoking while western countries were in later stages of smoking.
Reiss, Sauzet, Razum, Breckenkamp, and Spallek (2014) did a similar study where they compared the prevalence of smoking among Turkish immigrants who had emigrated to Germany and the Netherlands. They used two sets of data to come up with their findings. The first set of data was the German 2009 micro-census, while the second set of data was the Dutch POLS database. They also developed logistic regression models for age-specific smoking habits and sex-specific smoking behaviors. Generally, the researchers found that the immigrants had changed their smoking behaviors to suit those of their host nations (Reiss et al., 2014).
The strength of the adaptation was correlated with their length of stay. This relationship was stronger for Turkish immigrants who had left their country of origin before reaching 18 years. These findings support the views of similar researchers in this paper who have shown that the length of stay in immigrant countries often affects the health habits of immigrant groups.
Printz (2015) conducted another study to investigate the effect of immigration and acculturation on smoking among Latino and Asian immigrants in America. The researchers used a sample of 3,249 Latino and Asian immigrants and found that male immigrants smoked four times more than their female counterparts did (Printz, 2015). This finding could be translated to mean that male immigrants smoked 2.5 more cigarettes per day than their female counterparts did. These findings were also consistent with other studies that showed that the length of stay in the host country was a strong moderating factor for smoking habits among immigrants because Printz (2015) found that increased length of stay often leads to the increased frequency and prevalence of smoking among the sampled population. Their findings also showed that immigrants who acculturated themselves well, in terms of English proficiency and citizenship acquisition benefitted from reduced smoking behavior.
Li, Kwon, Weerasingh, Rey, and Trinh-Shevrin (2013) also arrived at the same finding when they explored the impact of smoking on Asian communities living in New York because they established that acculturation explained the consistent rise in smoking behavior among these immigrants, while the rate of smoking in the general population decreased. These findings were developed through an analysis of data from the REACH US Risk Factor Survey (2009-2011).
Gorman, Lariscy, and Kaushik (2014) also explored the role of acculturation in predicting the smoking behaviors of immigrants in the US after finding that female immigrant smoke less than their male counterparts do. They found that gender had a moderating effect on acculturation because differences in smoking behaviors between the sexes could not be holistically explained by acculturation alone (Gorman et al., 2014). They came up with this finding after analyzing data from 3,249 Latino and Asian immigrants living in the US.
Bostean, Ro, and Fleischer (2017) investigated smoking trends among US-born and foreign-born Latino immigrants and found that the latter group smoke less compared to the former. The findings of this paper would be helpful in understanding the disparities in smoking behaviors among foreign-born and US-born immigrants. Poureslami, Shum, and FitzGerald (2015) explored the reasons why Chinese immigrants in Vancouver continued smoking and found that their cultural inclinations provided less internal incentive to stop smoking. Cultural orientation can influence health behaviors like smoking.
In an article titled, “Immigrant Advantage,” Kolker (2013) says that Americans could learn how to reduce the incidence of diseases, such as asthma, by emulating the dietary practices and discipline that some immigrants exude from their culture. The authors drew attention to the high incidence of smoking and alcoholism in America as significant contributors to asthma cases in the country.
In a study to investigate the impact of the nativity on the relationship between asthma and immigrants, Arsen (2013) investigated the influence of a person’s immigration status on their risk of developing asthma. This study was prepared against a background of research studies that showed immigrants had better health outcomes than their host populations and the understanding (among many sociology researchers) that immigrants had poor SES and were more prone to asthmatic attacks, compared to host populations, which are ordinarily in higher SES (Alkerwi et al., 2012). The analysis of Arsen (2013) supported the findings of other studies in this paper, which showed that immigrants suffered a lower risk of asthmatic attacks compared to the native-born population. He conducted this study by comparing the risk of asthma among French immigrants and the native population.
Lee, O’Neill, Ihara, and Chae (2013) also explained the importance of understanding how long immigrants have stayed in their host countries, as a prerequisite for understanding their health outcomes, because they explained that although acculturation improves the SES of immigrants, their continued stay in the host countries is associated with worsening health outcomes. The researchers developed these findings after conducting a cross-sectional study that used data from a survey analyzing the behaviors of immigrants who came to the host nations between 2003 and 2004. Their findings implied that increased stay in the US often leads to the adoption of unhealthy lifestyle behaviors, which are responsible for poor health outcomes (Lee et al., 2013).
Relevant Factors Identified in the Literature Review
As evidenced by this literature review, there is increased attention to understanding the effect of asthma and smoking among immigrant communities, not only in America but around the world as well. This concern is partly caused by the rising prevalence of asthma and associated complications, globally. Most of the researchers in this literature review have explored the causal pathway of asthma and allergies. However, there have been contradictory and conflicting findings regarding the interplay between allergy and the socioeconomic determinants of health. Immigration status is at the top of the list of factors that have been poorly understood, but as seen from this literature review, many researchers have tried to explain it.
The focus on socioeconomic status was an important theme of this literature review because I am focusing on African immigrants whose health has been proved to be affected by their socioeconomic conditions. I have also explored the role of acculturation on the smoking habits of immigrants and found that the longer the immigrants stayed in the host countries, the higher their intensity and frequency of smoking. I have established that there are significant gender differences in acculturation among different immigrant communities that would ultimately affect their general smoking behaviors.
While these studies (generally) have good merit in the way they were designed, I did not come across any study that focused on African immigrants as a unique sample population. In fact, the only studies that were close to our target population were those that sampled the health outcomes of African-Americans. However, these two populations are not the same. Additionally, the latter is not an immigrant group, per se. Based on this fact, there is a significant gap in the literature because health studies have failed to recognize the unique socio-cultural and economic dynamics of African immigrants that affect their health. This study seeks to fill this research gap by investigating the association between smoking and asthma incidences among adult African immigrants in California.
Definitions
- Asthma (Dependent variable) – A respiratory condition characterized by the presence of spasms in the nasal cavity. It often causes difficulty in breathing and inflammation of the lungs. Some common symptoms include wheezing, coughing, and shortness of breath (Arsen, 2013).
- Smoking (Independent variable) – The inhalation of tobacco smoke through the burning of cigarettes. Smoking is often a behavioral issue characterized as a recreational drug habit (Dutra et al., 2014).
- Socio-ecological Model (SEM) – A model for understanding the interaction between personal and ecological effects of human behavior. The model is often used to identify behavioral and organizational leverage points that could be used to improve human health outcomes (Jayasinghe, 2015).
- California Health Interview Survey (CHIS) – One of the largest health surveys in the USA that provides population-based, standardized health-related data for California. The data is often obtained from 58 counties in California and is collected using telephone surveys (UCLA Center for Health Policy Research, 2017).
- Socioeconomic status – Socioeconomic status is the classification or the positioning of the social and economic standing of a person or group, relative to other populations. The social and economic metrics for classification could be influenced by people’s education standards, income, and work experience (Carroll, 2013).
- Immigration status – This concept refers to the legal status of American immigrants. Immigrants may assume several legal statuses, including (but not limited to) permanent residency, green card holders, and resident aliens, all of which allow people who are not born in the US to live in the country legally. The process of gaining an immigrant status is often a lengthy and complex one. This fact explains why people often need thorough consultations with an immigration attorney before seeking a legal status (Reingle et al., 2014).
Assumptions
According to Whaley (2014), assumptions are things that are believed to be true, but cannot be verified by the researcher. One key assumption in this study is that the findings from the California Health Interview Survey are credible and reliable. I believe that this information is free from errors because the dataset forms the bedrock of our research findings. I also assume that the findings obtained in this study are representative of all African immigrants in California, regardless of their social or cultural affiliations.
Some of the assumptions highlighted above affect the choice of using the CHIS database as the main source of data. More importantly, in the context of this research, we assume that the CHIS database is a credible and reliable source of information. Indeed, I have confidence that this database will provide the most credible and reliable information because it is the most comprehensive health survey in the state (UCLA Center for Health Policy Research, 2017).
Additionally, the survey is based on a broad-based research strategy that includes the views of more than 20,000 respondents hailing from different counties in the state (UCLA Center for Health Policy Research, 2017). The credibility of using the database is also derived from the fact that the CHIS data have been successfully used to inform clinical health research, cancer research and formulate policies at institutional levels (UCLA Center for Health Policy Research, 2017). These facts are important in affirming the credibility of this study because the more the database has been used to inform other research studies, the higher its credibility and reliability in the context of this research review.
Scope and Delimitations
One factor that could have been important to the current study, but was excluded from it, was primary research to investigate the relationship between smoking and asthma among the target population. I did not include primary research because the study scope is statewide. Conducting statewide research could have required many resources and a lot of time that I did not have (Creswell, 2014). Consequently, relying on CHIS data was a better option. Another issue that could have been pertinent to this research is contextualizing the research problem to include African-Americans as part of the target population. However, I could not do so because, although African-Americans are an immigrant group in California, they have unique social, political, and economic dynamics that are different from those of Africans, who were the target population.
Lastly, it would have been prudent to include secondary research data from other CHIS databases in this study because the data used in this report only apply to a survey conducted in 2015. Integrating previous CHIS databases would have helped to provide a long-term view of the research problem. However, I could not do so because the process could have taken a lot of time and resources, especially in integrating the two sets of data (Creswell, 2014). Furthermore, the data analysis process would have taken a long time to complete and possibly delayed the submission of this research study.
Limitations of the Study
According to Mangal and Mangal (2013), limitations of a study often refer to issues that are outside a researcher’s control. One key limitation of my study is that the findings obtained are limited to the time (or period) the data presented in the California Health Interview Survey (CHIS) was collected. The use of secondary research data in this paper comes with different limitations for me as the researcher, including limiting the information used to publicly available data.
Similarly, the use of the CHIS data limits me to the current measurements used in the dataset, thereby constraining my ability to undertake a historical review of the same data because measurement standards often change periodically (Bowling, 2014). Lastly, since this study uses co-relational studies, it comes with different limitations that include the difficulty of understanding which variable leads to a change in the other. In this regard, it would be difficult to understand causation from the use of this design. These factors outline the limitations of the study.
Significance of the Study
The findings of the proposed study would help to fill the research gap identified above by identifying unique attributes about Californian African immigrants that may affect the relationship between asthma and smoking. Findings could help to formulate health interventions that address these attributes to achieve the highest levels of success in reducing the rates of asthma cases. Moreover, the findings of this study could help health experts to develop focused interventions that appeal to unique African immigrant dynamics as a strategy to minimize the effects of smoking on the overall health of the African immigrants.
The findings of the proposed study could also contribute to the professional practice by informing policy decisions about smoking and outlining the mediating factors affecting the relationship between this variable with asthma. Mistakes made in the past highlight this fact because it took up to 50 or 60 years of research on tobacco use before governments started implementing policy decisions that reflected their findings (Pattanayak, Sunita, & Anshu, 2016). The proposed research could provide a reliable basis for the formulation of public health decisions affecting asthma management through an understanding of its relationship with smoking.
Lastly, the findings of the proposed study would help to promote positive social change by reducing the asthma attacks nationwide because African immigrants are among the worst affected, but one of the understudied groups. Exploring the relationship between the independent variable (smoking) and other mediating factors and the dependent variable (asthma), within this demographic, would be the first step in managing the disease and decreasing associated morbidity and mortality. Comprehensively, health care service providers might be able to have a holistic approach to asthma management that will consider all immigrant groups and not just the frequently studied ones – Asian and Hispanic immigrants.
Summary and Conclusion
In this section, I have shown that researchers have investigated the relationship between smoking and asthma. Particularly, they have demonstrated that these two variables share a positive relationship because increased smoking often increases asthma incidences. Their findings have also shown that smoking often causes irritation along the air pathways, thereby leading to asthma. Similarly, they have also shown that the smoking habit damages hair-like structures (cilia) along the air pathways, leading to an exacerbation of the asthma condition. This data has often been presented as a general relationship between smoking and asthma.
Specialized studies have often focused on age differences and income groups to explain the same relationship. Those that have further broken down the demographic divide have investigated the relationship between smoking and asthma among specific immigrant groups such as Hispanics and Asians. The relationship between smoking and asthma among African immigrants is a relatively under-researched area because studies have always neglected this immigrant group.
I seek to fill this research gap by exploring the relationship between smoking and asthma among adult African immigrants using a quantitative correlational study design. The main variables for this study are smoking as the independent variable and asthma as the dependent variable. My main source of data will be the California Health Interview Survey (CHIS) dataset. Ii hopes that this research will result in a better understanding of the association between smoking and asthma among adult African immigrants in California. The findings of this study could have a positive impact on social change because they could help to reduce the impact of asthma within the target population. Furthermore, they could inform policy decisions affecting the research issue.
References
Abraído-Lanza, A. F., Echeverría, S. E., & Flórez, K. R. (2016). Latino immigrants, acculturation, and health: promising new directions in research. Annual Review of Public Health, 37, 219–236.
Acton, A. (2012). Bronchial diseases: Advances in research and treatment. New York, NY: Scholarly Editions. Web.
Alkerwi, A., Sauvageot, N., Pagny, S., Beissel, J., Delagardelle, C., & Lair, M. L. (2012). Acculturation, immigration status and cardiovascular risk factors among Portuguese immigrants to Luxembourg: Findings from ORISCAV-LUX study. BMC Public Health, 12, 864. Web.
Allem, J. P., Ayers, J. W., Unger, J. B., Irvin, V. L., Hofstetter, C. R., & Hovell, M. F. (2012). Smoking Trajectories among Koreans in Seoul and California: Exemplifying a common error in age parameterization. Asian Pacific Journal of Cancer Prevention : APJCP, 13(5), 1851–1856. Web.
Amer, M., & Awad, G. (2015). Handbook of Arab-American psychology. London, UK: Routledge. Web.
American Academy of Allergy, Asthma & Immunology. (2017). Asthma statistics. Web.
Arcury, T.A., Summers, P., Carrillo, L., Grzywacz, J.G., Quandt, S. A., & Mills, T. H. (2014). 3rd Occupational safety beliefs among Latino residential roofing workers. American Journal of Industrial Medicine, 57(6), 718–725.
Arsen, E. (2013). La vie avec l’asthme: Analysis of asthma susceptibility differences between immigrant and native populations in France. New York, NY: Columbia University Academic Commons. Web.
Barr, R. G., Avilés-Santa, L., Davis, S. M., Aldrich, T. K., Gonzalez, F., Henderson, A. G., … Smith, L. J. (2016). Pulmonary disease and age at immigration among Hispanics. Results from the Hispanic community health study/study of Latinos. American Journal of Respiratory and Critical Care Medicine, 193(4), 386–395.
Becerra, B. J., Scroggins, C. M., & Becerra, M. B. (2014). Association between asthma and obesity among immigrant Asian Americans. California health interview survey, 2001–2011. Preventing Chronic Disease, 11, 1–5. Web.
Beck, A. F., Simmons, J. M., Huang, B., & Kahn, R. S. (2012). Geomedicine: Area-based socioeconomic measures for assessing risk of hospital reutilization among children admitted for asthma. American Journal of Public Health, 102(12), 2308–2314.
Benchimol, E. I., Manuel, D. G., To, T., Mack, D. R., Nguyen, G. C., Gommerman, J. L., … Guttmann, A. (2015). Asthma, type 1 and type 2 diabetes mellitus, and inflammatory bowel disease amongst South Asian immigrants to Canada and their children: A population-based cohort study. PLoS ONE, 10(4), 6–5. Web.
Borges, G., Orozco, R., Rafful, C., Miller, E., & Breslau, J. (2012). Suicidality, ethnicity and immigration in the United States. Psychological Medicine, 42(6), 1175–1184. Web.
Bosdriesz, J. R., Lichthart, N., Witvliet, M. I., Busschers, W. B., Stronks, K., & Kunst, A. E. (2013). Smoking prevalence among migrants in the US compared to the US-born and the population in countries of origin. PLoS ONE, 8(3), 1–13.
Bostean, G., Ro, A., & Fleischer, N. L. (2017). Smoking trends among U.S. Latinos, 1998–2013: The impact of immigrant arrival cohort. International Journal of Environmental Research and Public Health, 14(3), 1–12. Web.
Bowling, A. (2014). Research methods in health: Investigating health and health services. London, UK: McGraw-Hill Education (UK). Web.
Braback, L., Vogt, H., & Hjern, A. (2011). Migration and asthma medication in international adoptees and immigrant families in Sweden. Clinical and Experimental Allergy, 41(8), 1108-1115. Web.
Burgess, D. J., Mock, J., Schillo, B. A., Saul, J. E., Phan, T., Chhith, Y., … Foldes, S. S. (2014). Culture, acculturation and smoking use in Hmong, Khmer, Latinos, and Vietnamese communities in Minnesota. BMC Public Health, 14, 791. Web.
Cabieses, B., Uphoff, E., Pinart, M., Antó, J. M., & Wright, J. (2014). A systematic review on the development of asthma and allergic diseases in relation to international immigration: The leading role of the environment confirmed. PLoS ONE 9(8), 1–10.
Camacho-Rivera, M., Kawachi, I., & Bennett, G. G. (2015). Revisiting the Hispanic health paradox: The relative contributions of nativity, country of origin, and race/ethnicity to childhood asthma. J Immigrant Minority Health, 17(3), 826–833. Web.
Carroll, K. (2013). Socioeconomic status, race/ethnicity, and asthma in youth. American Journal of Respiratory and Critical Care Medicine, 188, 1180–1181.
CDC. (2014). NCEH state fact sheets: California.
CDC. (2015). Current smoking among adults in 2015 (Nation).
Celedón, J. (2016). Achieving respiratory health equality: A United States perspective. New York, NY: Humana Press. Web.
Chiu, M., Lebenbaum, M., Lam, K., Chong, N., Azimaee, M., Iron, K., … Guttmann, A. (2016). Describing the linkages of the immigration, refugees and citizenship Canada permanent resident data and vital statistics death registry to Ontario’s administrative health database. BMC Medical Informatics and Decision Making, 16, 135. Web.
Cho, J. H., & Paik, S. Y. (2016). Association between electronic cigarette use and asthma among high school students in South Korea. PLoS ONE, 11(3), 1–13. Web.
Corlin, L., & Brugge, D. (2014). The hidden asthma epidemic in immigrant subpopulations. Web.
Corlin, L., Woodin, M., Thanikachalam, M., Lowe, L., & Brugge, D. (2014). Evidence for the healthy immigrant effect in older Chinese immigrants: A cross-sectional study. BMC Public Health, 14, 603–607. Web.
Coutts, C. (2016). Green infrastructure and public health. London, UK: Routledge. Web.
Creswell, J. (2014). Research design: Qualitative, quantitative, and mixed methods and approaches (3rd ed.). Thousand Oaks, CA: SAGE Publications, Inc. Web.
Currie, G., & Baker, J. (2012). Asthma. Oxford, UK: OUP Oxford. Web.
Dutra, L. M., Williams, D. R., Gupta, J., Kawachi, I., & Okechukwu, C. A. (2014). Human rights violations and smoking status among South African adults enrolled in the South Africa Stress and Health (SASH) study. Social Science & Medicine, 105, 103–111.
Elk, R., & Landrine, H. (2012). Cancer disparities: Causes and evidence-based solutions. New York, NY: Springer Publishing Company. Web.
Fenelon, A. (2013). Revisiting the Hispanic paradox in the United States: The role of smoking. Social Science & Medicine, 19(82), 1–9.
Findley, S., & Matos, S. (2015). Bridging the gap: How community health workers promote the health of immigrants. Oxford, UK: Oxford University Press, Incorporated. Web.
Flynn, M. A., Carreón, T., Eggerth, D. E., & Johnson, A. I. (2014). Immigration, work, and health: A literature review of immigration between Mexico and the United States. Revista de Trabajo Social, 6, 129–149. Web.
Fox, M., Entringer, S., Buss, C., DeHaene, J., & Wadhwa, P. D. (2015). Intergenerational transmission of the effects of acculturation on health in Hispanic Americans: A fetal programming perspective. American Journal of Public Health, 105(3), 409–423. Web.
Garcia-Marcos, L., Robertson, C., Anderson, R., Ellwood, P., Williams, H., Wong, G., …ISAAC Phase Three Study Group. (2014). Does migration affect asthma, rhinoconjunctivitis and eczema prevalence? Global findings from the international study of asthma and allergies in childhood. International Journal of Epidemiology, 43(6), 1846–1854.
Gatrell, A., & Elliott, S. (2014). Geographies of health: An introduction. London, UK: John Wiley & Sons. Web.
Gilioli, G., Caroli, A. M., Tikubet, G., Herren, H. R., & Baumgärtner, J. (2014). Implementation of a socio-ecological system navigation approach to human development in Sub-Saharan African communities. Journal of Public Health Research, 3(1), 218.
Gilreath, T. D., Chaix, B., King, G., Matthews, S., & Flisher, A. J. (2012). Multi-level influence of school norms on tobacco use in South Africa: An ecometric consideration of group differences. Cancer Causes & Control : CCC, 23(1), 27–36.
Gong, T., Lundholm, C., Rejnö, G., Mood, C., Långström, N., & Almqvist. C. (2014). Parental socioeconomic status, childhood asthma and medication use – a population-based study. PLoS ONE 9(9), 106-110.
Gorman, B., Lariscy, J., & Kaushik, C. (2014). Gender, acculturation, and smoking behavior among U.S. Asian and Latino immigrants. Social Science & Medicine, 106, 110–118.
Grzywacz, J. G., Arcury, T. A., Mora, D., Anderson, A. M., Chen, H., & Rosenbaum, D. A. (2012). Work organization and musculoskeletal health: Clinical findings from immigrant Latino poultry processing and other manual workers. J Occup Environ Med., 54(8), 995–1001.
Guest, G. (2014). Public health research methods. London, UK: SAGE Publications. Web.
Guruge, S., Birpreet, B., & Samuels-Dennis, J. (2015). Health status and health determinants of older immigrant women in Canada: A scoping review. Journal of Aging Research, 2(5), 1–12.
Hamilton, E., Cardoso, J., Hummer, R., & Padilla, Y. (2011). Assimilation and emerging health disparities among new generations of U.S. children. Demographic Research, 25(25), 781–818. Web.
Hegde, D. (2015). Essays on research methodology. New York, NY: Springer. Web.
Im, E. O., Rendell Endowed, M. O., Chang, S. J., Chee, W., Chee, E., & Mao, J. (2015). Immigration transition and depressive symptoms: Four major ethnic groups of midlife women in the U.S. Health Care for Women International, 36(4), 439–456.
Jacobsen, K. (2016). Introduction to health research methods. New York, NY: Jones & Bartlett Publishers. Web.
Jayasinghe, S. (2015). Social determinants of health inequalities: Towards a theoretical perspective using systems science. International Journal for Equity in Health, 14, 71–73.
Kapp, J., Simoes, E., DeBiasi, A., & Kravet, S. (2016). A conceptual framework for a systems thinking approach to us population health. Systems Research and Behavioral Science, 3(4), 98–105. Web.
Keet, C. A., McCormack, M. C., Pollack, C. E., Peng, R. D., McGowan, E., & Matsui, E. C. (2015). Neighborhood poverty, urban residence, race/ethnicity and asthma: rethinking the inner-city asthma epidemic. The Journal of Allergy and Clinical Immunology, 135(3), 655–662.
Kelly, N., Glick, D., Kulbok, P., Clayton, L., & Rovnyak, V. (2012). Health status of migrant farmworkers in the Shenandoah valley. J Community Health Nurs., 29(4), 214–224.
Kolker, C. (2013). The immigrant advantage: What we can learn from newcomers to America about health, happiness and hope. New York, NY: Simon and Schuster. Web.
Landsbergis, P.A., Grzywacz, J.G., & LaMontagne, A.D. (2014). Work organization, job insecurity, and occupational health disparities. Am J Ind Med., 57(5):495–515. Web.
Lee, P. N., Forey, B. A., & Coombs, K. J. (2012). Systematic review with meta-analysis of the epidemiological evidence in the 1900s relating smoking to lung cancer. BMC Cancer, 12, 385. Web.
Lee, S., O’Neill, A. H., Ihara, E. S., & Chae, D. H. (2013). Change in self-reported health status among immigrants in the United States: Associations with measures of acculturation. PLoS ONE, 8(10), 56-61.
Li, S., Kwon, S. C., Weerasingh, I., Rey, M. J., & Trinh-Shevrin, C. (2013). Smoking among Asian Americans: Acculturation and gender in the context of tobacco control policies in New York City. Health Promotion Practice, 14(5), 18–28.
Lopez, L., & Golden, S. H. (2014). A new era in understanding diabetes disparities among U.S. Latinos–all are not equal. Diabetes Care, 37(8), 2081–2083.
Loue, S. (2013). Handbook of immigrant health. New York, NY: Springer Science & Business Media. Web.
Mahmoudi, M. (2016). Allergy and asthma: Practical diagnosis and management. New York, NY: Springer. Web.
Mangal, S., & Mangal, S. (2013). Research methodology in behavioural sciences. New York, NY: PHI Learning Pvt. Ltd. Web.
Marshall, T. (2016). Public opinion, public policy, and smoking: The transformation of American attitudes and cigarette use, 1890–2016. New York, NY: Rowman & Littlefield. Web.
Martinez, O., Wu, E., Sandfort, T., Dodge, B., Carballo-Dieguez, A., Pinto, R., … Chavez-Baray, S. (2015). Evaluating the impact of immigration policies on health status among undocumented immigrants: A systematic review. Journal of Immigrant and Minority Health / Center for Minority Public Health, 17(3), 947–970. Web.
Moore, L., de Silva-Sanigorski, A., & Moore, S. N. (2013). A socio-ecological perspective on behavioural interventions to influence food choice in schools: Alternative, complementary or synergistic? Public Health Nutrition, 16(6), 1000–1005.
Moreland-Russell, S., & Brownson, R. (2016). Prevention, policy, and public health. Oxford, UK: Oxford University Press. Web.
Naturopath, C. (2013). Asthma solved naturally: The surprising underlying causes and hundreds of natural strategies to beat Asthma. New York, NY: Logical Books. Web.
Okechukwu, C. A., Souza, K., & Davis, K. D. (2014). Discrimination, harassment, abuse, and bullying in the workplace: contribution of workplace injustice to occupational health disparities. American Journal of Industrial Medicine, 57(5), 573–586.
Onono, M., Kwena, Z., Turan, J., Bukusi, E. A., Cohen, C. R., & Gray, G. E. (2015). “You know you are sick, why do you carry a pregnancy again?” Applying the socio-ecological model to understand barriers to PMTCT service utilization in western Kenya. Journal of AIDS & Clinical Research, 6(6), 467. Web.
Pattanayak, S., Sunita, P., & Anshu, S. (2016). Role of Cd4+T cell sub-populations in allergic asthma: A new strategy of natural flavonoids to ameliorate asthma. New York, NY: GRIN Verlag. Web.
Pichardo-Geisinger, R., Mora, D. C., Newman, J. C., Arcury, T. A., Feldman, S. R., & Quandt, S. A. (2014). Comorbidity of tinea pedis and onychomycosis and evaluation of risk factors in Latino immigrant poultry processing and other manual laborers. South Med J., 107(6), 374–379.
Polosa, R., Caponnetto, P., & Sands, M. (2012). Caring for the smoking asthmatic patient. The Journal of Allergy and Clinical Immunology, 130(5), 1221–1224.
Poureslami, I., Shum, J., & FitzGerald, M. (2015). Why do Chinese people with COPD continue smoking: The attitudes and beliefs of Chinese residents of Vancouver, Canada? Diversity and Equality in Health and Care, 12(1), 18–27.
Printz, C. (2015). Immigration associated with an increase in smoking among Latinos, Asians. American Cancer Society, 121(1), 3–5. Web.
Reed, H., & Barosa, G. (2016). Investigating the refugee health disadvantage among the U.S. immigrant population. Journal of Immigration and Refugee Studies, 15(1), 1–10.
Reingle, J. M., Caetano, R., Mills, B. A., & Vaeth, P. A. C. (2014). The role of immigration age on alcohol and drug use among border and non-border Mexican Americans. Alcoholism, Clinical and Experimental Research, 38(7), 2080–2086. Web.
Reiss, K., Razum, O., & Lehnhardt, J. (2015). Factors associated with smoking in immigrants from non-western to western countries – what role does acculturation play? A systematic review. BioMed Central, 13(11), 1–10. Web.
Reiss, K., Sauzet, O., Razum, O., Breckenkamp, J., & Spallek, J. (2014). How immigrants adapt their smoking behavior: Comparative analysis among Turkish immigrants in Germany and the Netherlands. BioMed Central, 14, 844–48. Web.
Rhodes, S. D., Mann, L., Simán, F. M., Song, E., Alonzo, J., Downs, M., … Hall, M. A. (2015). The impact of local immigration enforcement policies on the health of immigrant Hispanics/Latinos in the United States. American Journal of Public Health, 105(2), 329–337. Web.
Riosmena, F., Wong, R., & Palloni, A. (2013). Migration selection, protection, and acculturation in health: A binational perspective on older adults. Demography, 50(3), 1039–1064. Web.
Ro, A. (2014). The longer you stay, the worse your health? A critical review of the negative acculturation theory among Asian immigrants. International Journal of Environmental Research and Public Health, 11(8), 8038–8057. Web.
Rottem, M., Geller-Bernstein, C., & Shoenfeld, Y. (2015). Atopy and asthma in migrants: The function of parasites. Int Arch Allergy Immunology, 167, 41–46. Web.
Rumrich, I. K., & Hänninen, O. (2015). Environmental asthma reduction potential estimates for selected mitigation actions in Finland using a life table approach. International Journal of Environmental Research and Public Health, 12(6), 6506–6522. Web.
Schenker, M., Casta–eda, X., & Rodriguez-Lainz, A. (2014). Migration and health: A research methods handbook. Oakland, CA: University of California Press. Web.
Shani, M., Band, Y., Kidon, M., Segel, M., Rosenberg, R., Nakar, S., … Vinker, S. (2013). The second generation and asthma: Prevalence of asthma among Israeli born children of Ethiopian origin. Respiratory Medicine, 107, 519–523.
Sharma, M. (2016). Theoretical foundations of health education and health promotion. London, UK: Jones & Bartlett Publishers. Web.
Sheikh, A., Steiner, M. F. C., Cezard, G., Bansal, N., Fischbacher, C., Simpson, C. R., … SHELS researchers. (2016). Ethnic variations in asthma hospital admission, readmission and death: A retrospective, national cohort study of 4.62 million people in Scotland. BMC Medicine, 14, 3. Web.
Spears, M., McSharry, C., Chaudhuri, R., Weir, C. J., De Wet, C., & Thomson, N. C. (2013). Smoking in asthma is associated with elevated levels of corticosteroid resistant sputum cytokines—an exploratory study. PLoS ONE 8(8), 1–10.
Sternberg, R. M., Nápoles, A. M., Gregorich, S., Paul, S., Lee, K. A., & Stewart, A. L. (2016). Development of the stress of immigration survey (SOIS): A field-test among Mexican immigrant women. Family & Community Health, 39(1), 40–52. Web.
Streja, L., Crespi, C. M., Bastani, R., Wong, G., Jones, C., Bernert, J., … Tashkin, J. (2014). Can a minimal intervention reduce secondhand smoke exposure among children with asthma from low-income minority families? Results of a randomized trial. Journal of Immigrant Minority Health, 16, 256–264. Web.
Tamimi, A., Serdarevic, D., & Hanania, N. (2012). The effects of cigarette smoke on airway inflammation in asthma and COPD: Therapeutic implications. Respiratory Medicine, 106, 319–328. Web.
Thakur, N., Oh, S. S, Nguyen, E. A., Martin, M., Roth, L. A., Galanter, J., … Meade, K. (2013). Socioeconomic status and childhood asthma in urban minority youths: The GALA II and SAGE II studies. American Journal of Respiratory and Critical Care Medicine, 188(10), 1202–1209.
UCLA Center for Health Policy Research. (2017). California Health Interview Survey (CHIS). Web.
UNICEF. (2016). Understanding the social ecological model (SEM) and communication for development (C4D). Web.
Walters, D. (2015). California anti-smoking drive cut rates in half. Web.
Whaley, B. (2014). Research methods in health communication: Principles and application. London, UK: Routledge. Web.
World Health Organization. (2016). Prevalence of tobacco smoking.
Yakob, B., & Ncama, B. P. (2016). A socio-ecological perspective of access to and acceptability of HIV/AIDS treatment and care services: A qualitative case study research. BMC Public Health, 16, 155. Web.