Abstract
Retinitis pigmentosa is a congenital eye defect that affects the retina and gradually progresses leading to impaired vision. The disease manifests when there is the deterioration of the retinal pigment, epithelium, and cone photoreceptors. Numerous effective diagnostic techniques for the disease exist, but unfortunately, there is no remedy for reversing the disease state or halting the progression of the disease. As a result, the disease has had negative effects on patients including segregation and stigmatization. This research, therefore, employed the qualitative approach in investigating the impact of retinitis pigmentosa on different aspects of the patients’ lives. The results indicated that patients with retinitis pigmentosa encounter a lot of stigma and discrimination in their socio-economic lives, with friends and family being the major discriminators. Due to a lack of awareness of the disease and under-sensitization, people have further ostracized patients with retinitis pigmentosa making them live in a state of solitude and suffering from depression.
Introduction
Retinitis pigmentosa (RP) is the major cause of acquired blindness in the developed world. The etiology of RP is due to mutations, including X-linked, and either autosomal dominant or recessive (Rehman, 2015). So far, researchers have identified over 200 mutations causing RP in over 100 different genes (Parmegiannii, 2011). Degeneration of the retina usually commences with the degradation of rods photoreceptors leading to nyctalopia. Continual worsening of the retina results in the formation of the ring-shaped scotoma in the middle of the margin, which can, in turn, spread to the macula and boundary. As the disease progresses, it causes the cone receptors to deteriorate, ultimately causing reduced vision.
Though genetic variation exists among RP patients, they present the same signs and symptoms. Globally, patients with RP affects 1 in 2500-7000 people aged between 20-60 years with histopathology in all forms of the disease being the shortening of outer parts of the rod (Parmeggiani, 2011). These statistics are based on clinical diagnostic techniques for retinitis pigmentosa employed when there is a family history of the disease, existence of nyctalopia, changes in retinal pigment, contraction of the visual field, and a decrease in the normal full-field electroretinograms (ERGs) among others (Mitamura et al., 2012). Defective ERGs exist before the onset of disease with amounts of ERGs and the size of fields of visions reducing exponentially. The diagnosis techniques include ophthalmoscopy, electroretinography, spectral ocular coherence tomography (OCT), and fluorescein angiography.
Problem statement
Despite advancements in science and understanding of the Retinitis pigmentosa disease, no evidence-based treatment exists (Parmeggiani, 2011). Consequently, RP patients have continued to suffer from research findings averring that cases of stigmatization and discrimination exist in several countries, especially at work (Spiegel, De Bel, & Steverink, 2015). These findings underscore the need to investigate further the challenges bedeviling RP patients. Since RP patients are a minority and due to rampant discrimination against them by members of the population, they are withdrawn and suffer in silence. Probing their plight and subsequently disseminating the resultant information is the first step to improving their lives.
Literature review
Patients with retinitis pigmentosa initially experience night blindness, then contraction of visual fields and eventually loss of primary vision in the latter stages of the disease (Manes et al., 2015). Due to visual impairment, RP patients contend with many difficulties in their daily existence. They have problems finding people in public places, lavatories, and even means of transportation, in the advanced form of the disease. Since they were able to do these things earlier, they have problems asking for help and tend to hide their condition and avoid social gatherings or events. These challenges generally stem from a lack of awareness of the disease by a majority of the people.
Socially, they grapple with exclusion by family and friends and face segregation in public places (Southwell, 2012). They are dependent on people to help them do many of their daily activities and so discrimination has a negative toll on them. The propensity to discriminate arise from societal norms and ideologies, and in some cases, school and media, and tend to influence most people’s attitudes. In Sweden, the law affords disabled people including those with visual problems, financial and social system support from the government. However, care providers such as ophthalmologists do not recognize RP and so cannot extend these services to RP patients. Additionally, the blind in Sweden have access to special taxis, but those with RP do not access them. Discrimination has thus led to solitude and depression due to reduced social contacts.
Economically, RP patients experience difficulties finding employment (Southwell, 2012). Out of the fear of discrimination, people ailing from retinitis pigmentosa tend to hide their disease status (Spiegel, De Bel, &Steverink (2015). Additionally, there is a high probability of people suffering from retinitis pigmentosa losing their jobs. This is highly likely due to mental instability. In their study on the mental health of people with retinitis pigmentosa, Sarah et al. (2013) discovered that RP patients have poor mental health compared to normal people. The contributing factors to mental instability include elevated levels of stress, depression, and suicidal thoughts. Furthermore, RP patients retire prematurely (Gao et al., 2015). This has serious economic consequences since they retire at the economically viable age. The result is that the retirees are likely to live in squalor when faced with discrimination.
Other problems RP patients are personal problems including; low self-esteem, fear of losing a job, difficulties planning for the future, being misunderstood and mistrusted, fear of being judged by normal people, especially when using the white cane (Southwell, 2012). The use of the white cane is usually a clear indication of a visually impaired person, and because of lacking understanding of retinitis pigmentosa, people are quick to judge RP patients. In Iran and Sweden, RP patients have expressed their unwillingness to use the white cane.
Aside from the above challenges, misdiagnosis of retinitis pigmentosa is another challenge the patients are grappling with. Misdiagnosis of the disease, especially in the early stages is a common occurrence (Yin et al., 2016). In Sweden and Iran, RP patients have blamed the wrong diagnosis, especially during childhood for their predicaments. They uphold the notion that perhaps with the proper diagnosis, doctors could have reversed their condition. This school of thought has many patients disillusioned and full of resentment for oculists.
Methodology
The research adopted a cross-sectional study design. The researchers quantified the qualitative data initially collected to know the extent of specific observations. The study population was patients with retinitis pigmentosa who attended checkups in various hospitals with names undisclosed in line with the ethical requirement of confidentiality. The sampling technique used was convenience sampling since the sample included only the people diagnosed with RP, who willingly contributed to the study. The data collection method was semi-structured interviews with the research questions being the effect of RP and vision loss on their socio-economic well-being, how they were managing the disease and if they participated in activities to better their lives. The ethical consideration of informed consent and confidentiality were highly considered throughout the study. The researchers collected data for academic purposes and participants remained anonymous. Study participants were at liberty to terminate their participation at any point throughout the study and were under no form of coercion.
Data Analysis
In data analysis, the research transformed qualitative data into quantitative and used descriptive statistics. The analyzed data was then presented using tables and a pie chart as shown below.
Table 1: Personal challenges RP patients’ experience.
Table 2: The number of RP victims participating in activities to improve their condition.
Table 3: How RP patients are managing their condition.
Table 4: The source of discrimination and the number of RP patients discriminated against.
Discussion of findings
Amongst the personal challenges, finding a spouse (20%), finding a job (45%), and interacting with people (35%) are major personal challenges that RP patients faced. These problems are due to low self-esteem, a psychological problem observed by Sarah et al. (2013). Finding a job, a spouse, and interacting with people are highly social activities, and therefore, feeling ‘unloved’ dictates social aspects of RP patients’ lives. The discovery that a third (75%) of the RP patients do not engage in any activities meant to improve their condition, such as forming a group to advocate for their rights, is worrying. It is in accord with the postulation of Spiegel, De Bel, and Steverink (2015) that RP sufferers fear socialization. Non-participation stems out of stigma and under-sensitization of RP. They are afraid nobody will care to listen to them and so trying to assert their essence in society appears to be an effort in futility.
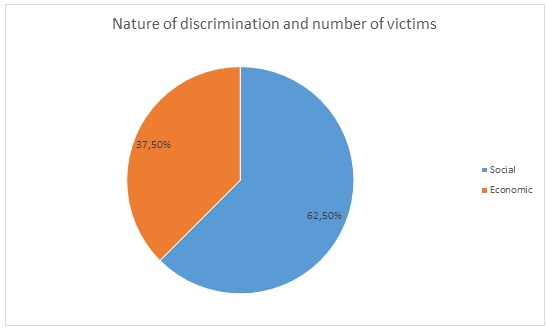
A majority of the respondents (75%) managed their condition by moving from the countryside to urban areas to minimize night blindness (37.5%) and took vitamin A (37.5%). Only 25% of RP patients used the white cane in managing their condition. Southwell (2012) documents the fear of RP patients using the white cane. Normally, RP patients fear that people will be quick to judge them as ‘disabled’, based on previous experiences. Social discrimination accounted for the greatest source of segregation at 62.5% while economic discrimination accounted for 37.5%. Southwell (2012) avers that family and friends, followed by public places, exclude RP sufferers more. A high level of social discrimination is thus commensurate to the discovery that the major discriminators are friends and family (62.5%) while the government was intermediate at 25%. Discrimination emanates from the lack of understanding of retinitis pigmentosa.
Conclusion
The plight of people suffering from retinitis pigmentosa is due to segregation and stigmatization. The society needs to be enlightened on the disease to eliminate the negative perceptions they have about it. Key in achieving this is the government’s involvement in a mass sensitization campaign and enforcing the laws guarding against discrimination of disabled people. Print and electronic media should also continually, highlight the plight of RP patients to reduce people’s ignorance. Additionally, there should be stronger social networks to support victims of RP.
References
Gao, G., Ouyang, C., Dai, J., Xue, F., Wang, X., Zou, L.,… Yu, M. (2015). Baseline traits of patients presenting at low vision clinic in Shanghai, China. BMC Ophthalmology, 15(16), 1-6.
Manes, G., Guilaumie, T., Vos, W., Devos, A., Audo, I., Zeitz, C.,… Hamel, C. (2015). High prevalence of PRPH2 in autosomal dominant retinitis pigmentosa in France and characterization of biochemical and clinical features. American Journal of Ophthalmology, 159(2), 302- 314.
Mitamura, Y., Mitamura- Aizawa, S., Nagasawa, T., Katome, T., Eguchi, H., & Naito, T. (2012). Diagnostic imaging in patients with retinitis pigmentosa. Journal of Medical Investigation, 59(1), 1-11.
Parmeggiani, F. (2011). Clinics, epidemiology and genetics of retinitis pigmentosa. Current Genomics, 12(4), 236-237.
Rehman, H. (2015). Retinitis pigmentosa. New Zealand Journal of Medicine, 128(1415), 54-55.
Sarah, K., Dong-Wook, S., Reum, A., Hyung, L., Hyock, P., Heon, P.,… Ki, L. (2013). Mental health of people with retinitis pigmentosa. Optometry and Vision Science, 90(5), 488-493.
Spiegel, T., De Bel, V., & Steverink, N. (2015). Keeping up appearances: the role of identity concealment in the workplace among adults with degenerative eye conditions and its relationship with well-being and career outcomes. Disability and Rehabilitation, 38(7), 627-636.
Southwell, P. (2012). The psychosocial challenge of adapting to visual impairment. British Journal of Visual Impairment, 30(2), 108-114.
Yin, X., Yang, L., Chen, N., Cui, H., Zhao, L., Feng, L.,… Li, G. (2016). Identification of CYP4V2 mutation in 36 Chinese families with Bietti crystalline corneoretinal dystrophy. Experimental Eye Research, 146(2), 154-162.