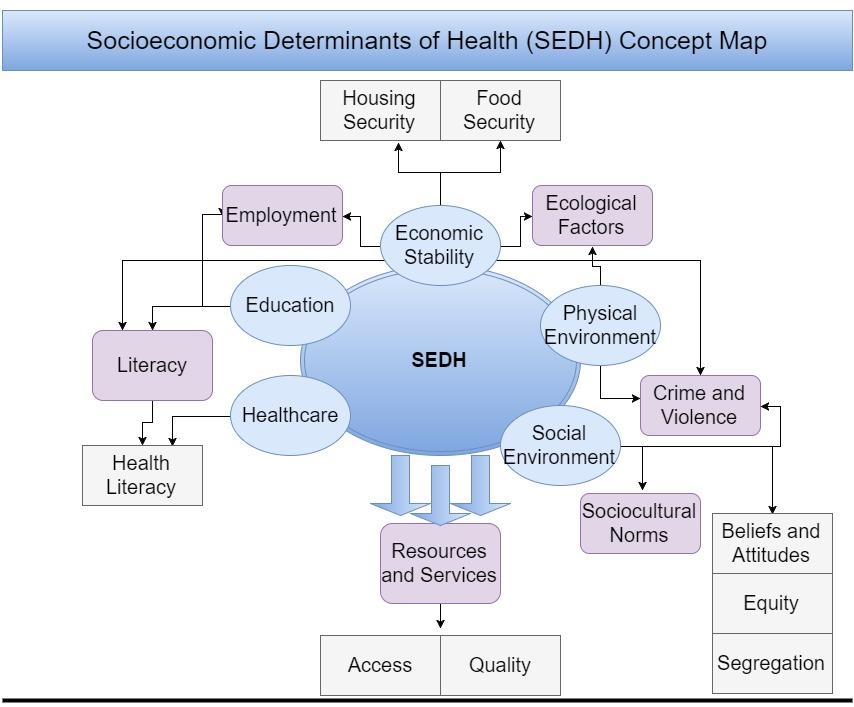
Figure 1 demonstrates an example of a concept map for the socioeconomic determinants of health (SEDH), which is based on the information from the Healthy People 2020 project (Office of Disease Prevention and Health Promotion [ODPHP], 2014). The map attempts to demonstrate the fact that there are complex interrelations between various social and economic factors and highlights the key elements of SEDH that ODPHP (2014) proposes to take into account.
SEDH is a complex of multiple factors that tend to affect health and can promote or limit the ability of medical healthcare to improve it. Together with other determinants of health, SEDH develops an even more complicated structure, which should be taken into account by healthcare specialists (Braveman & Gottlieb, 2014; Meyer, Castro-Schilo, & Aguilar-Gaxiola, 2014). In the figure, the five major elements of SEDH that are proposed by ODPHP (2014) (physical and social environment, education and health, economic stability) are shown to influence and co-influence various factors. For example, exposure to crime and violence is shown to be affected by the physical environment; however, the figure also demonstrates that economic and social environments can have an impact on it as well. The presented diagram does not intend to fully expose all the nuances of the interrelationship between the exceedingly complex factors, but it attempts to summarize the information provided by ODPHP (2014) and systematize it in a meaningful way.
The diagram also illustrates the idea that the five elements appear to have an impact on a very important health determinant: resources and services. Indeed, the physical environment affects the availability and quality of resources and services (Bircher & Kuruvilla, 2014). The social environment can influence the attitudes and mindset of people, prompting them to either seek out or refuse to seek out healthcare-related resources. For example, the existence of safe sex culture in a community can urge its members to obtain means of protection (Brown, O’Donnell, Crooks, & Lake, 2014). Also, discrimination and disparities can be important limiting factors in getting crucial resources (Mosquera, González-Rábago, Bacigalupe, & Suhrcke, 2017), and they are a part of the social environment of a person. Education and economic stability seem to co-influence each other (Braveman & Gottlieb, 2014; Mosquera et al., 2017), affecting people’s access to resources: economic stability is correlated with better educational opportunities, which, in turn, contribute to future economic stability that results in improved access to resources. On the other hand, poverty is also known to restrict access to education (and healthcare) (Bircher & Kuruvilla, 2014, p. 374). As for the healthcare element, it can incorporate, for example, local or national policies, which can be beneficial or restrictive.
The information is relevant for public health, and it should also be taken into account during community or individual health assessments (Meyer et al., 2014). Indeed, the determination of socioeconomic issues can help to design policies and community and individual interventions (Meyer et al., 2014; Mosquera et al., 2017). The information can be obtained directly from people during individual assessments; also, the observation and appropriate research of themselves or their neighborhoods can extend the knowledge. In the case of community assessment, governmental reports, research, and observation can be useful. Some of the factors that are mentioned in Figure 1 can be modified: for example, the lack of literacy or health literacy culture can be adjusted through educational means. Other factors need to be taken into account when determining the intervention: for instance, economic instability and limited access to resources prompts the use of more cost-effective means. Thus, the employment of a comprehensive assessment, which is supposed to include socioeconomic factors, is capable of customizing care and making it more effective (Bircher & Kuruvilla, 2014).
References
Bircher, J., & Kuruvilla, S. (2014). Defining health by addressing individual, social, and environmental determinants: New opportunities for health care and public health. Journal of Public Health Policy, 35(3), 363-386. Web.
Braveman, P., & Gottlieb, L. (2014). The social determinants of health: It’s time to consider the causes of the causes. Public Health Reports, 129(1), 19-31.
Brown, G., O’Donnell, D., Crooks, L., & Lake, R. (2014). Mobilisation, politics, investment and constant adaptation: lessons from the Australian health-promotion response to HIV. Health Promotion Journal Of Australia, 25(1), 35. Web.
Meyer, O., Castro-Schilo, L., & Aguilar-Gaxiola, S. (2014). Determinants of mental health and self-rated health: A model of socioeconomic status, neighborhood safety, and physical activity. American Journal of Public Health, 104(9), 1734-1741.
Mosquera, I., González-Rábago, Y., Bacigalupe, A., & Suhrcke, M. (2017). The impact of fiscal policies on the socioeconomic determinants of health. International Journal of Health Services, 47(2), 189-206.
Office of Disease Prevention and Health Promotion. (2014). Social determinants of health.