Introduction
In the recent decades, the issue of childhood obesity in the US has been increasingly coming to the forefront in the public view and in academia as a major health problem. Currently, the obesity rate in the States is some of the highest in the world, with a significant percentage of children being either simply overweight or outright obese as well.
Background and Significance of the Problem
One of three children in the US has excess weight issues, with obese children making up about 17 percent of the total population between the ages of 2 to 19 (Ogden, Carroll, Kit, & Flegal, 2014). It has been estimated that the numbers have grown to be seen as propagating unhealthy eating habits, coupled with lack of physical activity and other detrimental factors. These include uninhibited advertising of unhealthy (junk) foods in schools, high in calories, salt, sugar and fat, while healthier foods, high in nutrients, have a negligible presence in the advertisement scene. Communities are not equipped to educate children about the dangers of less healthy foods and the importance of a healthy lifestyle. They are often not equipped for active physical activity, and actively discourage it through absence of parks or safe roots for walking or biking. Similarly, community centers and child centers do not have unifying federal regulations and guidelines for healthy food promotion, and many community shops and retailers focus on unhealthy foods, decreasing the availability and affordability of healthy foods.
Obesity is strongly connected with a number of severe short and long-term health risks. These risks include increased cholesterol and blood pressure, which leads to higher risks of cardiovascular maladies, development of type 2 diabetes, breathing problems, and obesity later in life. There are also numerous problems related to the quality of living, which include low-esteem, negative perception of the quality of life, problems with social integration, all leading to psychological stress and depression (Childhood Obesity Causes & Consequences, 2015).
Statement of the Problem and Purpose of the Study
Despite the fact that reduction of childhood obesity is the target of many public health initiatives, with the Centers for Disease Control and Prevention, the Institute of Medicine, the US Surgeon General, and the government actively funding interventions at both state- and community levels, the effects have been minor. No significant changes have been recorded in both children and adults in the years 2003 to 2012, with obesity rates remaining high (Ogden et al., 2014).
However, several states have shown some measure of success at fighting obesity, with Oregon showing a 32 percent decline in obesity in the years 2003-2007, currently holding the last place among other states for childhood obesity (Singh, Kogan, & Dyck, 2010). Notably, according to a 2010 assessment, almost half of the schools did not sell less healthy food altogether and prohibited promotion of sweets and junk foods and 11 percent always offered healthy options first, and
This research will aim to study the childhood obesity-reducing interventions implemented in different states, how effective they are compared to those implemented in Oregon, and can similar interventions be recreated in other states to address the issue.
Research Questions, Hypothesis, and Variables with Operational Definitions
Research Question
What kinds of community nursing interventions support effective reductions in childhood obesity rates?
Hypothesis: Research and Null
This paper will test the hypothesis that the community interventions used in Oregon can be replicated in other states to achieve the same results. The research hypothesis is that application of these interventions and regulations in schools and communities in other states will be followed by gradual reduction of obesity prevalence. The null hypothesis would be that these interventions do not influence the obesity rates in significant ways, and that other local conditions and factors need to be studied to determine the causes of weight reduction among children in Oregon, in order to develop best practices.
Identifying and Defining Study Variables
The independent variable in this experimental study is the community nursing intervention, aimed at the removal of the unhealthy food promotion in communities and schools in particular, and active promotion of healthier, more nutritious foods. The dependent variables are the childhood obesity rates in the studied states. To achieve the most efficient comparison, the researchers would need to replicate the level of implementation of these interventions in Oregon, the controlled variables. This will allow the researchers to assess the differences in intervention effectiveness under the same conditions, and thus potentially find other factors affecting the differences in results.
Operationalize Variables
To successfully aggregate data in a coherent and reliable manner, the researchers would need to operationalize their variables. The experiment will assess the dependent variable childhood obesity levels, which will be determined by calculating what percentage of children with the amount of extra weight more than 10 percent higher than their body weight. The independent variable will be based on the total percentage of schools and communities to have fully integrated the same initiatives as Oregon. Finally, the passage of time will be estimated in years, following the same methodology as other studies. This should provide the research with a reliable way of interpreting the effectiveness of the experiment.
Literature Review
The United States continues to have a high prevalence level of childhood obesity. As Ogden, Carroll, Curtin, Lamb, and Flegal (2010) posit, a “in 2007-08, obesity prevalence (with body mass index (BMI) greater than or equal to the 95th percentile of the CDC growth chart) was 19.6% for children between 6 to 11 years of age and 18.1% for adolescents aged 12 to 19 years” (p.242). Alongside the increased incidence rates of childhood obesity, the consumption of energy intake obtained from take-away foods from home and at restaurants that deal with fast foods has been increasing rapidly (Bauer, Larson, Nelson, Story, & Neumark-Sztainer, 2009).
Fast foods are closely associated with higher calorific intake, fats, poor nutrient intake, higher sodium intake, and higher BMI. Hence, they correlate positively to the witnessed cases of childhood obesity. For example, Niemeier, Raynor, Lloyd-Richardson, Rogers, and Wing (2006) attribute a higher weight gain to the increased fast food intake during the transition age from adolescent to adulthood. Therefore, childhood obesity in the US is attributed to poor eating habits and meager food choices among children. These factors are modifiable through contextual and environmental factors such as making healthy foods available, ensuring that only convenient and appealing healthy foods are promoted, and/or adjusting prices. These approaches replicate Oregon’s childhood obesity interventions, which have significantly contributed to a reduction of the health problem.
Food prices form an important factor that determines the degree of consumption of unhealthy foods, which are associated with high childhood obesity. Indeed, the prevalence of childhood obesity varies according to household income. In case of Oregon, low-income earners (those earning $15,000 or less) with obesity stands at 29.4% compared to 25.1% of those who earn more than $15,000 (Oregon Health Authority, 2015). Consequently, successful childhood obesity intervention programs in Oregon incorporate parents whereby they (programs) are moderated to reflect their household incomes.
Benchmarking from the case of Oregon, other states intervention programs should focus on increasing the affordability of healthy food alternatives. When dealing with the problem of childhood obesity, most states recognize the value of school and family-based treatment approaches as two important facets of community-centered intervention for childhood obesity. For example, Kothandan (2014) reviews the effectiveness of the two aspects of interventions for childhood obesity. Cases of childhood obesity in the US have been increasing within the last ten years. Currently, childhood obesity is now considered a major public health issue. Consequently, an effective intervention program is inevitable if the problem must be dealt with in an amicable manner. However, amid this important proposition, Kothandan (2014) reviews articles published between 2001 and 2010. The author does not report the confidence intervals that are necessary in specifying the most effective community-based intervention approach.
Childhood obesity is not only a problem of the United States. The World Health Organization notes that from 1990 to 2010, the prevalence of obesity among children rose from 4.2 percent to 6.7 percent in the developing nations (CDC, 2010). However, in the US, the situation is more serious with obesity of children of up to 19 years having tripled over the last two decades to arrive at a figure of nearly 20 % (CDC, 2010).
In 2007, about 5.2 million children in the United States had obesity (CDC, 2010). From the figures of 2003, this finding is an increase by 570,000 cases of childhood obesity. Te figure represents about 10 percent prevalence increase. From 2007, the rates are hardly getting down. This situation raises alarm for CDC to take up proactive measures to curtail more increments. To accomplish this goal, CDC has been conducting intensive campaigns to curtail the consumption of foods that make children add weight. The goal of the intervention strategy entails increasing the utilization of nutritious foods such as fruits and vegetables. This intervention is significant upon considering that overweight is associated with obesity. In particular, from 1976 to 1980, about 5 percent of people who belong to 2 to 19 years of age were obese. Surprisingly, from 1990 through 2006, this figure rose to about 16.3 percent. Obesity became even prevalent among very young people. In particular, according to CDC, by 2006, obesity among 2 to 5 years old reached 12.4 percent right from 5 percent (CDC, 2010).
CDC has recorded incidences of severe obesity in the course of the last two decades. For instance, in 2006, about 11 percent of people aged 2 to 9 years of age were found to be above 97 percentile of the BMI. CDC carried out a study to investigate risk behaviors among the youths in which obesity is highly prevalent among 9th to 12th graders. In 1999, the 9th to 12th graders who were obese was 10.7 percent. However, in 2007, this figure rose to 13.0 percent.
Statistical findings from 2009 to 2010 on childhood obesity indicate that despite the high sensitization on the menace of childhood obesity, the situation is not getting milder. For example, CDC (2010) reveals that between 2009 and 2010, 16.9 percent of adolescents and children in the US were obese. However, the prevalence of obesity between these two years was less among preschool children as compared to adolescents. Based on gender, as shown in figure 1, boys had a prevalence percentage of 18.6 while girls had an incidence entitlement of 15.0 percent by 2010 (CDC, 2010). Comparing this data with the 1999 to 2000 statistics, it is clear that the prevalence of obesity among boys increased by a margin of 4.6 percent from 1990-2000 to 2009-2010. In case of girls, it increased by a margin of 1.2 percent. This observation suggests that intervention programs should target boys and girls differently depending on the disparity in prevalence levels.
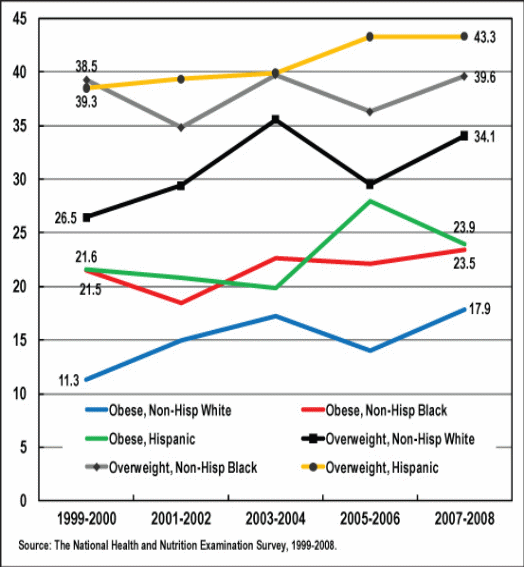
The US Department of Health and Human Services (HRSA) (2010) data depicts substantial disparities of the preference of obesity on racial grounds for children between the age of 10 and 17. Non-black Hispanic children had the highest prevalence level at 23.9 percent. Hispanic children followed closely at 23.4 percent (HRSA, 2010). American-Indians stood at 23.0 percent. Finally, Hawaiian children followed in terms of the racial disparity list at 20.9 percent (HRSA, 2010). Mixed race children had a preference rate of 14.2 percent while Asian children closed the racial disparity list at 8.7 percent. These variations suggest the need to adapt interventions to childhood obesity depending on the degree of risk for each group.
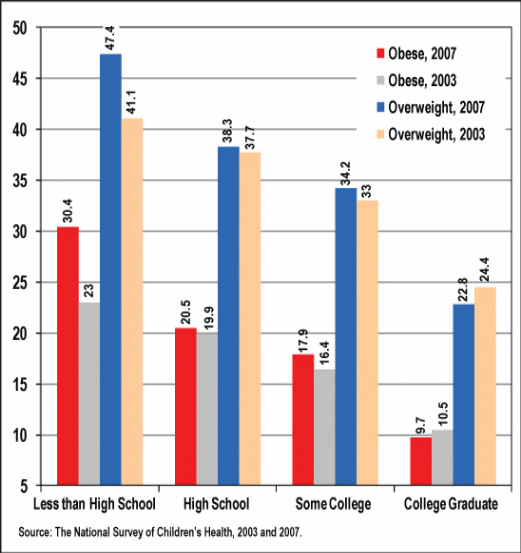
Differences in the prevalence of childhood obesity in terms of demographic aspects such as education within the last two decades, beginning from 1990 to 2010, among the US children is also evident. The data shows that the prevalence of obesity increased consistently with a decrease in household education from 2003 and 2007 as shown in figure 2. The US Department of Health and Human Services (2010) reckons, “the obesity prevalence for children with parents who have fewer than 12 years of education was 30.4 percent in 2007, 3.1 times higher than the obesity prevalence (9.7 percent) for children whose parents had a college degree” (p.3). This statistical findings show that the prevalence of childhood obesity had a direct relationship with parents’ educational levels.
Consistent with the literature review on the childhood obesity in the US, at the state level, for instance, the case of Oregon, obesity among children presents a serious health problem. For example, Oregon Health Authority (2015) reckons that about 33% of 6-9-year olds suffered from the health risk of obesity or overweight in 2012. About 15% of the children had obesity while 16% were overweight. Consequently, over the last three years, Oregon has incepted programs such as ensuring that Coordinated Care Organizations (CCOs) engage in screening, collection, and monitoring of children’s BMI. Oregon has also established nutrition standards program, obesity treatment plans, and comprehensive behavioral interventions that are aimed at reducing or checking weight loss through CCOs. Can these programs apply in other states to reduce the prevalence levels of childhood obesity depending on various demographic variables as discussed in the literature review? No research has been carried out to respond to this possibility. The research seeks to seal this gap.
Theoretical Framework
In any particular field of research, no one theoretical framework applies universally. In complex research endeavors such as the one that involves childhood obesity, the deployment of several frameworks is necessary in helping to develop an understanding of the required outcomes or the guiding interventions. The current research deploys the socio-environmental theoretical framework.
The choice of the framework stems from the primary concern of the research problem and various guiding propositions for the current research. For example, the research does not focus on individual health outcomes that are associated with childhood obesity. Rather, it focuses on population-based approaches to childhood obesity prevention and management. In such a context, Gibbs (2011) advises that the socio-environmental framework is the most appropriate. The framework is important where the ‘obesogenic’ environmental concept, including its implication on the obesity of the target population, is acceptable. Gibbs et al. (2011) asserts, “theoretical models that primarily address physical, policy, economic and socio-cultural environments, in addition to targeting psychosocial and behavioral factors, should be considered a guide for action” (p.105). The current research targets environmental change as a way of promoting a population’s behavioral change. In this context, the theoretical framework deployed in the research complies with the theory of health promotion consistent with the concerns of socio-environmental framework that is deployed in enabling schools to overcome various health problems. The theoretical framework is necessary in designing and guiding various health multi-level interventions. To this extent, the research will not only emphasize environmental changes, but also call upon for the involvement of communities in programs that address childhood obesity prevention and management. In so doing, individual and socio-cultural impacts, including the environmental implications of childhood obesity-related health outcomes, will be addressed.
Methodology
Sample
The research studies the kind of community nursing interventions that can effectively support the plan to reduce the rate of childhood obesity. The inclusion criteria for the interventions studied depend on four factors. Firstly, the intervention must focus on children between 2 and 14 years. Secondly, the intervention must be implemented in community or school-based settings where parents play important mediating roles for the children’s success. Fourthly, they should possess one or several aspects that define childhood obesity interventions that have been implemented in Oregon. All interventions implemented at local school level and not yet tested for compliance with the states’ guidelines for promoting health outcomes are excluded.
Setting
It is impossible to study all interventions in all states in America due to time and monetary resource constraints. Therefore, data is only collected in California and New Jersey. Hence, the research is done in the context of these two states compared to the state of Oregon.
Sampling Strategy
Simple random sampling is used as the method of getting the required sample. Hence, each element of the population bears an equal chance of being selected for the purposes of data collection. Five (5) interventions in each state are selected.
Research Design
The current research is designed as a primary study. Such a design requires the collection of first-hand data from the respondents (Saunders, Lewis, & Thornhill, 2009). After data collection, the research reviews and analyzes interventions that have been established to address the issue of childhood obesity in California and New Jersey. Quantitative data that will be extracted for comparison include the percentage decline of the prevalence of childhood obesity in the studied states compared to Oregon after the administration of various identified childhood obesity reduction interventions. Qualitative data collected will capture how people and institutions such as schools have received the interventions, including their perceptions of their (interventions) efficacy. The current research is designed as an experimental study. The rationale here is founded on the fact that the administration of childhood obesity prevention programs leads to modifications or manipulation of the participants’ behaviors.
References
Bauer, K., Larson, N., Nelson, C., Story, M., & Neumark-Sztainer, D. (2009). Fast food intake among adolescents: secular and longitudinal trends from 1999 to 2004. Preventive Medicine, 48(3), 284–287.
CDC. (2010). National Obesity. New York, NY: Centre for Diseases Control.
Childhood Obesity Causes & Consequences. (2015). Web.
Gibbs, L., Waters, E., Leger, L., Green, J., Gold, L, & Swinburn, B. (2011). A settings-based theoretical framework for obesity prevention community interventions and research. Australian and New Zealand Journal of Public Health, 35(2), 104-106.
Kothandan, S. (2014). School-based interventions versus family based interventions in the treatment of childhood obesity-a systematic review. Archives of public health, 72(3), 1-10.
Niemeier, H., Raynor, A., Lloyd-Richardson, E., Rogers, L., & Wing, R. (2006). Fast food consumption and breakfast skipping: predictors of weight gain from adolescence to adulthood in a nationally representative sample. Journal of Adolescent Health, 39(6), 842–849.
Ogden, C., Carroll, D., Curtin, L., Lamb, M., & Flegal, K. (2010). Prevalence of high body mass index in US children and adolescents, 2007-2008. Journal of the American Medical Association, 303(3), 242–249.
Ogden, C., Carroll, M. D., Kit, B. K., & Flegal, K. M. (2014). Prevalence of Childhood and Adult Obesity in the United States, 2011–2012. Survey of Anesthesiology, 58(4), 206. Web.
Oregon Health Authority. (2015). Recommended Strategies to Address Childhood Obesity. Oregon: Public Health Division.
Saunders, M., Lewis, P., & Thornhill, A. (2009). Research Methods for Business Students. New Jersey, NJ: Prentice Hall.
Singh, G. K., Kogan, M. D., & Dyck, P. C. (2010). Changes in State-Specific Childhood Obesity and Overweight Prevalence in the United States from 2003 to 2007. Arch Pediatr Adolesc Med Archives of Pediatrics & Adolescent Medicine, 164(7), 1-2.
The US Department of Health and Human Services (HRSA). (2010). Childhood Obesity in the United States, 1976-2008: Trends and Current Racial/Ethnic Social Economic and Geographic Disparities. Web.