Drug Misuse and Abuse
Addiction is a recurrent, chronic disorder characterized by compulsive substance seeking and use despite harmful consequences. Because it involves functional abnormalities in brain circuits involved in reward, stress, and self-control, it is classified as a brain condition. These alterations might remain for a long time after a person stops using drugs. It is very similar to other disorders like heart disease. Both interfere with an organ’s normal, healthy functioning, have substantial negative consequences, and are, in many circumstances, preventable and treatable. They can last a lifetime if left untreated and may even result in death.
Why do people use drugs? People use drugs for a variety of reasons and here are the common reasons:
- To be happy. Drugs can provide extremely pleasurable experiences. Following the initial pleasure, the medicine produces a variety of side effects. Stimulants such as cocaine, for example, produce sensations of strength, self-assurance, and increased energy. Opioids, such as heroin, produce euphoria, which is followed by feelings of relaxation and fulfillment.
- To feel better. Some persons with social anxiety, stress, or depression turn to medications to feel less anxious. Stress can play a substantial role in the initiation and maintenance of drug use and relapse in those who are addicted (return to drug use).
- To perform better. Some people are under pressure at school, work, or in sports to improve their attentiveness. This may impact your decision to try or continue using medications such as prescription stimulants or cocaine.
- Social pressure and curiosity. Teenagers are particularly vulnerable since peer pressure can be incredibly powerful. Adolescence is a stage of life when will accept risk factors such as drug-using peers, which can lead to substance abuse.
When people first use a drug, they may perceive what appear to be favorable effects. They might also believe they have complete control over how they use them. Drugs, on the other hand, have the ability to quickly take control of a person’s life. Other fun activities become less enjoyable as drug use continues, and the person is required to ingest the substance just to feel “normal” (Drug Misuse and Addiction, 2020). They are battling their drug addiction, despite it causing them and their loved ones significant problems. Some people may feel tempted to take more of a substance or to use it more frequently, even in the early stages of drug use, which are addiction signs.
Even modest drug use poses a risk. Consider how a drunk social drinker could get behind the wheel of a car and quickly turn a pleasurable activity into a life-threatening disaster. Occasional drug use, such as abusing an opioid to get high, can result in comparable undesirable outcomes, such as impaired driving and overdose. Another question arises: why do people continue to abuse drugs? Initially, taking medicines is usually a personal decision. Chronic use, on the other hand, can significantly reduce a person’s ability to exercise self-control. The loss of self-control is a hallmark of addiction. Physical changes in brain parts critical for judgment, decision-making, learning and memory, and action control occur in people with addiction. These alterations assist in explaining why addiction is so obsessive.
Can we determine whether a person can be a drug addict? Addiction, like other diseases and disorders, varies from person to person, and no single characteristic affects whether or not a person will become addicted to medications. In general, the more risk factors a person has, the more likely they are to take drugs and get addicted. On the other hand, protective factors lower a person’s risk. Both environmental and biological risks and protective factors exist.
Genes, developmental stage, and even gender or ethnicity are biological factors that can influence an individual’s predisposition to addiction. Genes account for 40 to 60% of a person’s risk of addiction, including the influence of environmental variables on gene expression, known as epigenetics (Drug Misuse and Addiction, 2020). Teenagers and adults with mental illnesses are also more susceptible to drug usage and addiction than others.
Factors Affecting Drug Addiction
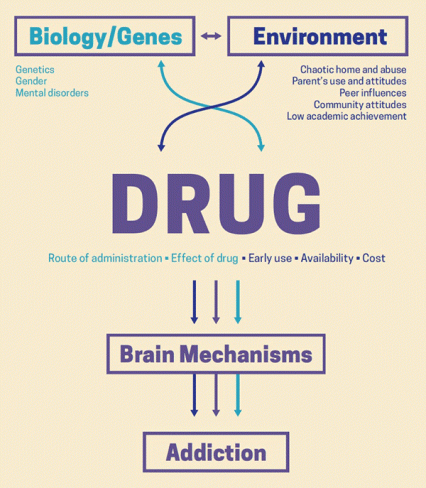
Environmental factors include family, friends, or other social relations of a person. To look closer at each factor separately:
- Family. The home environment is extremely crucial, especially throughout childhood. Parents or elder family members who abuse drugs and those who break the law can put their children at risk for future drug problems.
- Friends and Peers. During the teen years, friends and other peers might have a growing influence. Teens who use drugs can influence even those without risk factors to try drugs for the first time. A child’s struggles in school or a lack of social skills can enhance the likelihood of them using or becoming addicted to drugs.
Moreover, the age when a person starts using drugs affects their addiction. Even though drug use can lead to addiction at any age, the earlier people begin taking drugs, the more likely they are to develop serious problems. This could be related to the negative effects of medicines on the growing brain (Drug Misuse and Addiction, 2020). It could also be the result of a mix of early social as well as biological preconditions. For example, lack of stability in one’s home or family, physical or sexual abuse, genetics, or mental illness. Despite this, early use is a major predictor of future difficulties, including addiction. Therefore, drug abuse prevention requires constant parental monitoring and supervision. These skills can be improved by rule-making training, monitoring techniques, praise for good behavior, and gentle, persistent discipline that implements specified family norms. Drug education and information for parents and caregivers reinforce what children learn about the dangers of drugs and allow for family discussions on legal and illegal drug usage. Family-focused therapies for the general population can help improve specific parenting behaviors, lowering the likelihood of drug misuse later.
Aside from social interactions, prescriptions for medicines can be made with the right use of technology, which will help to avoid drug misuse and abuse. Prescription drug monitoring programs (PDMPs) are state-run electronic databases that track the prescribing and distribution of regulated prescription drugs to patients (Drug Misuse and Addiction, 2020). While evidence on the observable consequences of these programs is still scarce, the use of PDMPs has been associated with lower rates of opioid prescribing and overdose in some states; nonetheless, questions of best practices, ease of use, and interoperability remain unresolved. Interactive strategies like peer discussion groups and addressing issues with parents, which allow for active participation in learning about drug usage and reinforcing skills, are most effective in prevention programs.
Work Cited
“Drug Misuse and Addiction.” National Institute on Drug Abuse, 2020.