The broad category between health information systems
Many have high trust in health data innovation, or health IT. Healing centers plan to diminish restorative blunders, for example, requesting and controlling the wrong measurement of a medicine. Suppliers would share tolerant data effortlessly to improve health service delivery (Huston, 2013). Governments and organizations want to spare cash by enhancing effectiveness. However, health care specialists have not completely grasped these advances. A few specialists note that high health cost hinders technology advancement and research.
Some surveys recommend that actualizing health IT systems may ruin health care delivery. Thus, policymakers must be informed to support healthcare information systems. HIT envelops a wide cluster of new advances intended to oversee and share health-related data. The most essential kind of health records is a framework that electronically gathers stores and sorts out the patient’s history. Thus, an effective health information system will diminish medical blunders and enhance managerial productivity. The methods of collecting health records vary with location, objective, and population. However, health information systems could be an electronic health record (HER), or personal health records (PHR).
Electronic record frameworks arrive in an assortment of forms and proportions. Some gather and share persistent data just inside a specific foundation or inside a specific health institution, while others are incorporated into bigger data systems. The abilities of EHR frameworks and the degree to which they are coordinated in health care delivery fluctuate. EHR frameworks gather and store persistent information, stock patient information to physicians on solicitation, grant doctors to enter tolerant consideration requests, and help doctors in settling on proof-based clinical choices.
The computerized physician order entry is another health information system. The CPOE is a critical part of a completely useful EHR framework. This permits doctors to request medications and research facility tests digitally. Thus, wiping out blunders connected with obscured transcribed solutions. CPOE frameworks check for the exactness of solution requests, hailing any requests that seem great. One study presumed that CPOE frameworks for medicines could decrease preventable pharmaceutical mistakes by as much as 55 percent.
The four phases of health information systems
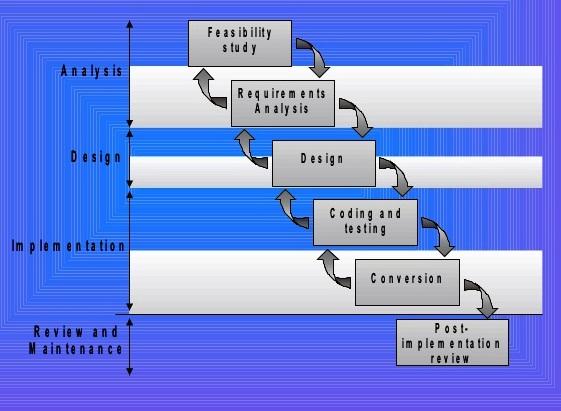
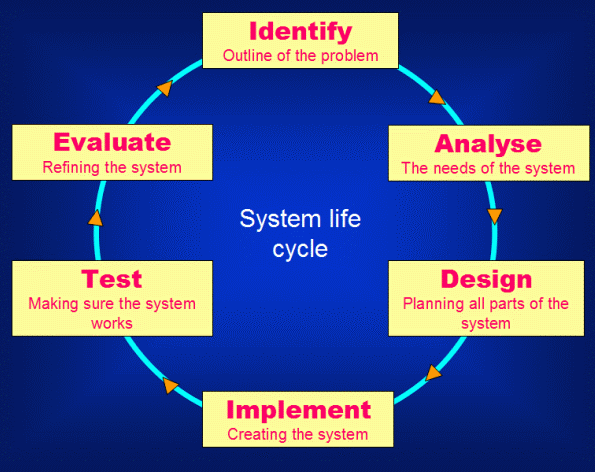
The phases of health information systems include analysis, design, implementation and, maintenance. Public health information frameworks are made to bolster the needs of certain project ranges, which include infant screening, birth deformities, inoculation, transferable infection reconnaissance, harm counteractive action, and bioterrorism (Lavin, Harper, & Barr, 2015). Information portals preserved by these projects are populated with information reported by health care workers.
These storehouses of health information send surveillance reports that are handcrafted to serve specific needs, which are not interoperable among health institutions. The absence of joining and interoperability arrangement prompts the wasteful utilization of assets and dissatisfaction among families and healthcare workers (Suter, Oelke, Adair, & Armitage, 2013). Thus, an effective health information system guarantees safe and reliable patient records. Consequently, HIT systems facilitate the integration of health care works and research institutions (Yen & Bakken, 2012).
The analysis phase covers the feasibility study and requirement analysis. The health analysis prepares a marshal plan for the design and implementation of the health information system. By implication, the analysis phase tackles the feasibility and requirement analysis of the EHR. The second phase provides the design, coding, and testing of the EHR. Please note that EHR design architecture facilitates the implementation phase (Wright & Sittig, 2014). The conversion of test analysis is carried out in the implementation phase. However, post-implementation activities are carried out in the maintenance phase.
Key elements in the needs assessment
Appraisal of health needs is not a procedure of listening to patients or depending on individual experience. However, it is a precise strategy for recognizing unmet health and social insurance needs of a populace and rolling out improvements to meet these unmet needs. It includes an epidemiological and subjective way to deal with deciding needs, which fuses clinical and cost viability. This methodology must adjust clinical, moral, and monetary contemplations of need. Health assessment needs to transcend the strategy for measuring diseases, but include an effective management plan.
The gap analysis is the initial step in the needs assessment. In this progression, issues are recognized and the contrasts between the present state and the perfect state are dissected. Once the whole investigation is finished, the critical step starts by deciding why the gap exists. Since assets are constrained, needs should be built up. Begin with the most imperative issue and work with the analysis. If patients are grumbling about administration quality issues and leaving the practice these issues will take need. Every practice must figure out which issues are most imperative and the manner they will be handled. It is a smart thought to catch evaluation discoveries in a report, which clears up issues and empowers the agreement
The implementation phase facilitates the HIT framework. Not all issues can be unraveled with an EHR. Issues such as poor preparation, staff with insufficient abilities, and ineffectual approaches and methods be regrettable with an EHR. Besides EHR contemplations, it is advisable to audit assets, administrative practices, and current arrangements. Needs appraisals are powerful instruments that facilitate health care development and performance. Needs evaluations can be exorbitant attempts that require substantial ventures of time and skill, however, they can be avoided.
HIT steering committee
A HIT controlling board needs to incorporate delegates from all partners. The controlling board of trustees separates authoritative limits, perceiving that the stream of data must be patient-oriented. The steering committee must have a lead representative that qualifies as a doctor or chief medical director. Consequently, a nurse, research representative, physician, government agent, legal unit, EHR consultant must be part of the steering committee.
The selection process
The strategy for selection must be based on the needs assessment of the health information system. By implication, the HIT system must reflect the challenge of the target group. Thus, members of the steering must understand their responsibilities. Doctors and medical caretakers will be the essential clients of EHR and need to comprehend and be occupied with the determination, usage, appropriation, and ideal utilization of EHR parts.
Team heads must have the capacity to lead the council with an impartial approach and have the capacity to give an ideal opportunity for members. The CFO or the central bookkeeper can help with surveying budgetary availability, distinguishing financing sources, incorporating the business, and arranging genius forma money related articulations for grants. An EHR specialist must explore numerous seller decisions and ventures in readiness, determination, and execution (Thede, 2015).
Training needs for end-users
The training needs depend on the assessment project. However, the assessment team must have basic computer skills. Consequently, a certified IT professional must be part of the steering committee. Members must be trained on the needs assessment to enhance performance. Feedback channels must be created to improve communication among team members.
References
Huston, C. (2013). The impact of emerging technology on nursing care: Warp speed ahead. The Online Journal of Issues in Nursing, 18(1), 34-45.
Lavin, M., Harper, E., & Barr, N. (2015). Health information technology, patient safety, and professional nursing care documentation in acute care settings. The Online Journal of Issues in Nursing, 20(2), 23-34.
Suter, E., Oelke, N., Adair, C., & Armitage, G. (2013). Ten key principles for successful health systems integration. Health Q., 19(3), 34–56.
Thede, L. (2015). Informatics: Electronic health records: A boon or privacy nightmare? The Online Journal of Issues in Nursing, 20(17), 234-345.
Wright, A., & Sittig, D. (2014). A four-phase model of the evolution of clinical decision support architectures. Int J Med Inform, 80(12), 621–749.
Yen, P., & Bakken, S. (2012). Review of health information technology usability study methodologies. J Am Med Inform Assoc. 19(3), 413–422.