Introduction
Disability is an omnipresent phenomenon in healthcare that embodies an array of conditions that limits one’s functioning. Due to the need of modern health care communities and societies to conceptualize disability in order to find methods of properly meeting the needs of people with disabilities, models of disability are essential. It is through theoretical frameworks that governmental entities, health care practitioners, and decision-makers, as well as individuals in society, will be equipped with the necessary knowledge and an objective perspective on impairment. Overall, disability is a complex issue that reaches far beyond the medical field. Indeed, social, cultural, political, economic, and environmental factors play an important role in conceptualizing disability, which is why it is essential to incorporate them in one complete theoretical model. This paper is designed to overview some of the models of disability, including medical and holistic models, to compare them with the International Classification of Functioning, Disability, and Health (ICF). The results of the comparative evaluation are anticipated to provide informative insights on the benefits ICF, as a new perspective on impairment, might contribute to contemporary practices related to managing disability at multiple levels.
ICF Model Description
Among the approaches to disability research and policy-making, there are several emerging models that have been developed by professionals in the field of health care to ensure consistency in all aspects of living with disabilities. One of such important models is ICF, proposed by the World Health Organization (WHO) as a framework for a complex view on disability. This framework provides several qualifiers for classifying diseases, health conditions, and disorders for effectively aiding people with treatment and assistance (WHO, 2002). This approach integrates two perspectives on disability, including medical and social models, neither of which is sufficient enough when applied separately. Therefore, ICF is a multifaceted framework that integrates both medical and social aspects of disability for effective diagnosis and policy implementation.
In particular, among the elements in the framework, the interconnection between which inherently involves the interplay of health conditions and contextual factors. In particular, ICF “identifies the three levels of human functioning classified by ICF: functioning at the level of body or body part, the whole person, and the whole person in a social context” (WHO, 2002, p. 10). Thus, the impairment at either of these levels might be labeled as a disability. Figure 1 demonstrates the diagram of the distribution of the model’s elements among the three levels.
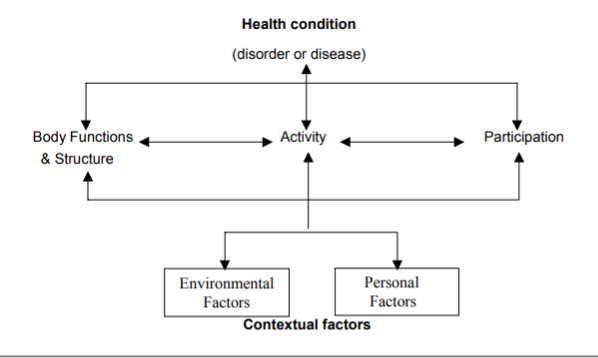
As the diagram shows, health condition represents disorders or diseases which involve particular diagnoses with malfunctioning of bodily systems. Disruptions in health at this level might negatively affect human performance in the social context. Body functions involve physiological and psychological performance, while body structures might be defined as “anatomical parts of the body such as organs, limbs and their components” (WHO, 2002, p. 10).
Activity is a concept that involves an individual’s ability to accomplish everyday tasks, while impairments might limit activity by obstructing the ability to cope with daily actions. Moreover, the social level also involves participation, which is “involvement in a life situation” that might be limited due to disability (WHO, 2002, p. 10). Finally, environmental factors include the life situation in which a person lives, while personal factors include demographic characteristics and individual particularities.
In such a manner, the combination of these factors predetermines how an individual experiences disability at different levels. Overall, the model provides the basis for analyzing disability at multiple levels of the life of an individual not to separate health condition from social context but to apply an integrative framework for enhanced wellbeing. Thus, when applying the model, the disability might be classified using several qualifiers depending on the level. The person’s functioning is evaluated on a scale from one to five for thorough classification (WHO, 2002). Indeed, at the level of body function and structure, the presence of impairment or injury is used as a qualifier. At the level of activity and participation, the decisive qualifiers are the performance qualifier and the capacity qualifier. Performance qualifier “describes what an individual does in his or her current environment,” while the capacity qualifier “describes an individual’s ability to execute a task or an action” (WHO, 2002, p. 11). At the contextual factor level, the individual’s life quality in a given environment is assessed. Thus, ICF is a multilevel framework that integrates all the manifestations of the disability.
Value of a More Holistic Model of Disability versus the Medical Model
To assess the value of the ICF model, one should compare it to other commonly used models in health care that view disabilities from a different angle. In particular, a holistic or affirmative approach and a medical approach might be used for the comparison. On a general scale, the development of ICF was based on the integration of the perspectives of several approaches to disability, which contributed to its completeness and flexibility. Therefore, such a characteristic implies that the medical model, which was one of the frameworks in ICF, might yield a more limited outlook on the issue at hand. Indeed, the medical model “views disability as a feature of the person, directly caused by disease, trauma or other health condition, which requires medical care provided in the form of individual treatment by professionals” (WHO, 2002, p. 8). Within the context of medicine, this model does not put an individual with a disability in a social context. Instead, the condition is viewed from the perspective of ableism, which implies perceiving a person with a disability as a dysfunctional human being.
More specifically, the medical model is based on the assumption that disability is the source of pain and suffering. Some researchers state that “the medical model encourages the simplistic view that disability is a personal tragedy for the individual concerned (Swain & French, 2000, p. 579). Such an approach separates the individual from society, his or her environment, and the personal factors that might play an important role in the diagnosis and management of the condition. Instead, the medical model limits one’s existence to the manifestation of only one level, which is body functions and structures. In comparison to ICF, the medical model is invalid and inefficient in yielding functional solutions for policy-making to meet the multilevel needs of people with disability. However, it is relevant to compare the ICF model with a more holistic one to draw conclusions about its anticipated effectiveness in addressing disability issues.
In particular, this holistic model might be referred to as an affirmative model. Similar to ICF, Swain and French (2000) propose this disability framework in opposition to the limited social and medical models. This approach allows for using a positive view of disability from the perspective of treatment and management opportunities and not mere concentration on the limitations and suffering. According to Swain and French (2000), the model “signifies the rejection of presumptions of tragedy, alongside rejections of presumptions of dependency and abnormality” (p. 578). It allows for setting disabled people in a general inclusive social setting without separating them. This framework is a holistic approach that incorporates multiple levels, especially the social one, of human life. However, it is less structured and less flexible in comparison to the ICF model. It lacks the classification and diagnosis basis that the ICF model introduces. Thus, the value of ICF is evident on the basis of the results of its comparison with other models.
Anticipated Benefits of ICF for Health Care Practices
Given the description of the ICF model and its structure, as well as its comparison to other models, one should identify the benefits that the implementation of ICF might provide for health care practices. At the level of policy-making, the ICF framework provides a comprehensive classification, which might help in accommodating policies in such sectors as transportation, education, employment, and others (WHO, 2002). Specific regulations and status-based adjustments for people with disabilities might be generated to ensure that the needs of this population are met. As for the influence on health care practice, based on ICF, health care interventions might be developed “to prevent or ameliorate limitations in person or societal level functioning by correcting or modifying intrinsic functions or structures of the body” (WHO, 2002, p. 8). Thus, the attention to individuals’ capacity and performance indicators might allow for better accommodation of medical practices to help people with disability to manage their conditions using contextual and activity-based factors.
Moreover, the ICF model implementation is likely to contribute to the economic analysis within the health care context. Indeed, according to WHO (2002), “determining whether resources are effectively used in health care … requires a consistent and standard classification of health and health-related outcomes that can be costed and compared internationally” (p. 7). Using the data on the burden of disability on individuals, communities, and societies, specific economic policies might be implemented to regulate resource allocation. Finally, research also benefits from the ICF model implementation due to the pull of issues and topics that require an evidential basis that might be retrieved using research results. Research activities in the field of disability using the ICF classification model might generate effective tools for comprehensive activity assessment of individuals with a disability.
Conclusion
In summation, the comparison and evaluation of the models of disability demonstrate that ICF has a significant value for the health care setting. The model integrates multiple levels of disability manifestations to ensure that individuals’ body functions and structure, activities, and contextual factors are combined to assess their needs. Unlike other models, ICF does not limit individuals’ lives to tragic and suffering experiences but rather finds ways to assist people in their normal functioning in society. Overall, the model provides a strong theoretical basis for development in the spheres of health care interventions, research, economic analysis, and policy-making. Therefore, it is recommended to implement this model of disability as an integral part of a new approach to diagnosing, classifying, and managing disability to ensure a shift in attitudes within social and institutional settings.
References
Swain, J., & French, S. (2000). Towards an affirmation model of disability. Disability & Society, 15(4), 569–582.
World Health Organization. (2002). Towards a common language for functioning, disability, and health ICF. Web.