While the requirements for healthy sleep vary from one person to another due to their schedule and the quality of life, considering sleep health in the context of a Healthy People 2020 objective is essential for addressing several limitations. One of the main issues associated with sleep health refers to the lack of public awareness and knowledge regarding the need for adequate sleep. Moreover, the treatment of sleep disorders is essential in order to improve the overall quality of life as well as facilitate safety, especially in terms of workplace settings and roads.
The adult population was chosen as the target for the healthcare problem due to the limited understanding of the importance of sleep for a healthy life. According to Avidan (2018). an average adult needs 7.5 to 8 hours of sleep per night; although, many people can function when sleeping for only 6 hours. Furthermore, sleep needs depend on a person and can extend to 9 and more hours per night.
During the move from adolescence into adulthood, patterns of sleep change. For instance, the majority of adults experience middle sleep, which is less restorative compared to slow-wave deep sleep. Therefore, the issue is essential to consider because poor sleep in adults is a widespread problem, with 25% of adults in the US only reporting insufficient sleep 15 out of 30 days (Healthy People 2020, 2020). The public health burden of poor sleep in adults also includes chronic sleep disorders as well as the decreased awareness that can lead to road and workplace accidents (Figure 1).
Demographic data concerning sleep health in adults suggests that the issue of poor sleep has a significant impact on the overall health of the adult population. According to the Healthy People 2020 (2020) findings, 32.8% of adults with obstructive sleep apnea sought medical evaluation between 2015 and 2016. This suggests that only a third of the population with sleep issues is educated enough on their health to seek medical evaluation.
The population aged 45-64 years gets the least sufficient sleep at night compared to other age groups (Figure 2). Furthermore, only 67.4% of adults (67. 5% males and 67.3% females) get sufficient sleep per night, with the Healthy People 2020 target rate being 72.8% (Healthy People 2020, 2020). Poor sleep should be addressed as the number of motor vehicle crashes due to drowsy drowning has increased to 2.9% in 2015, with the program’s target being 2.1% (Healthy People 2020, 2020).
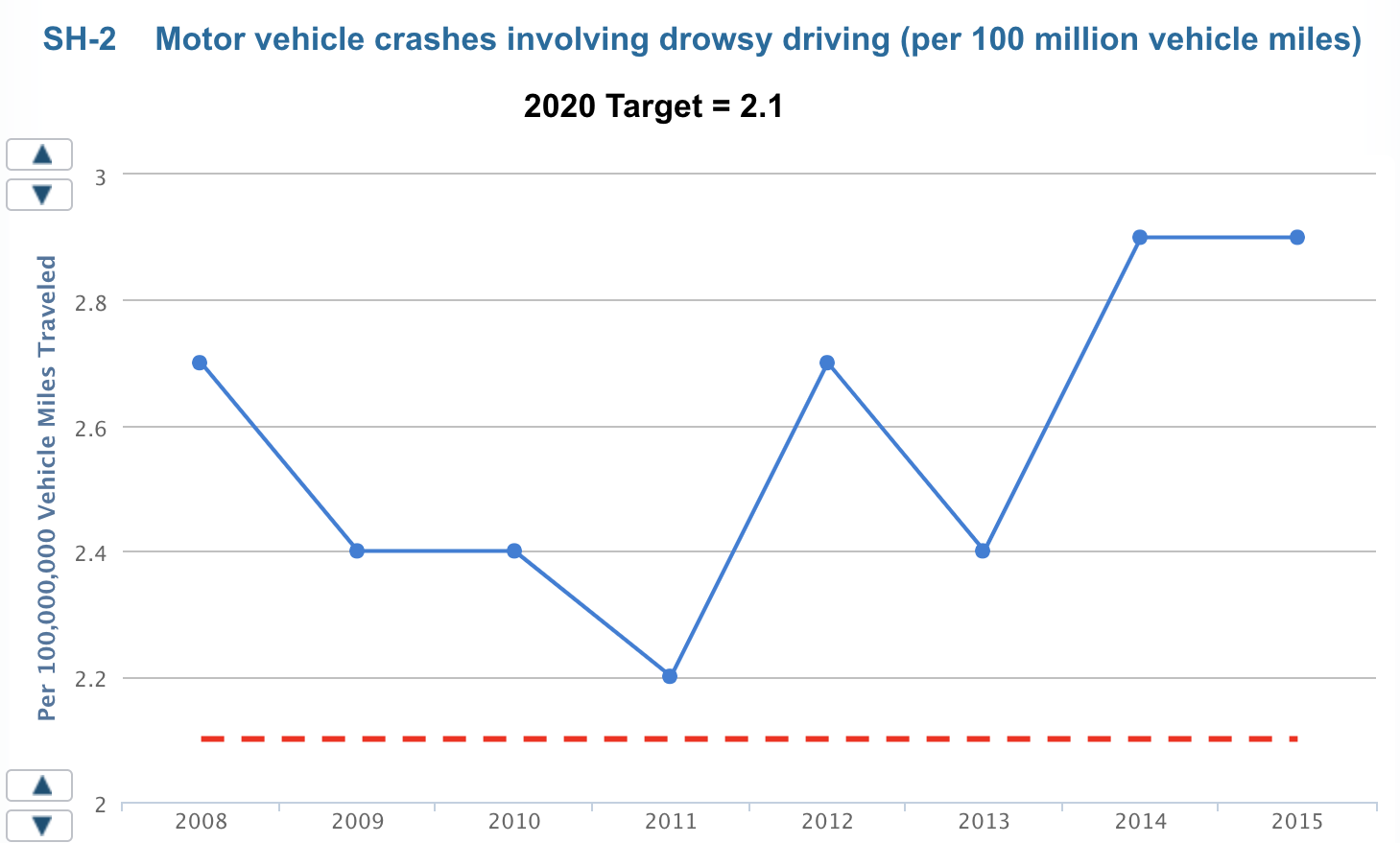
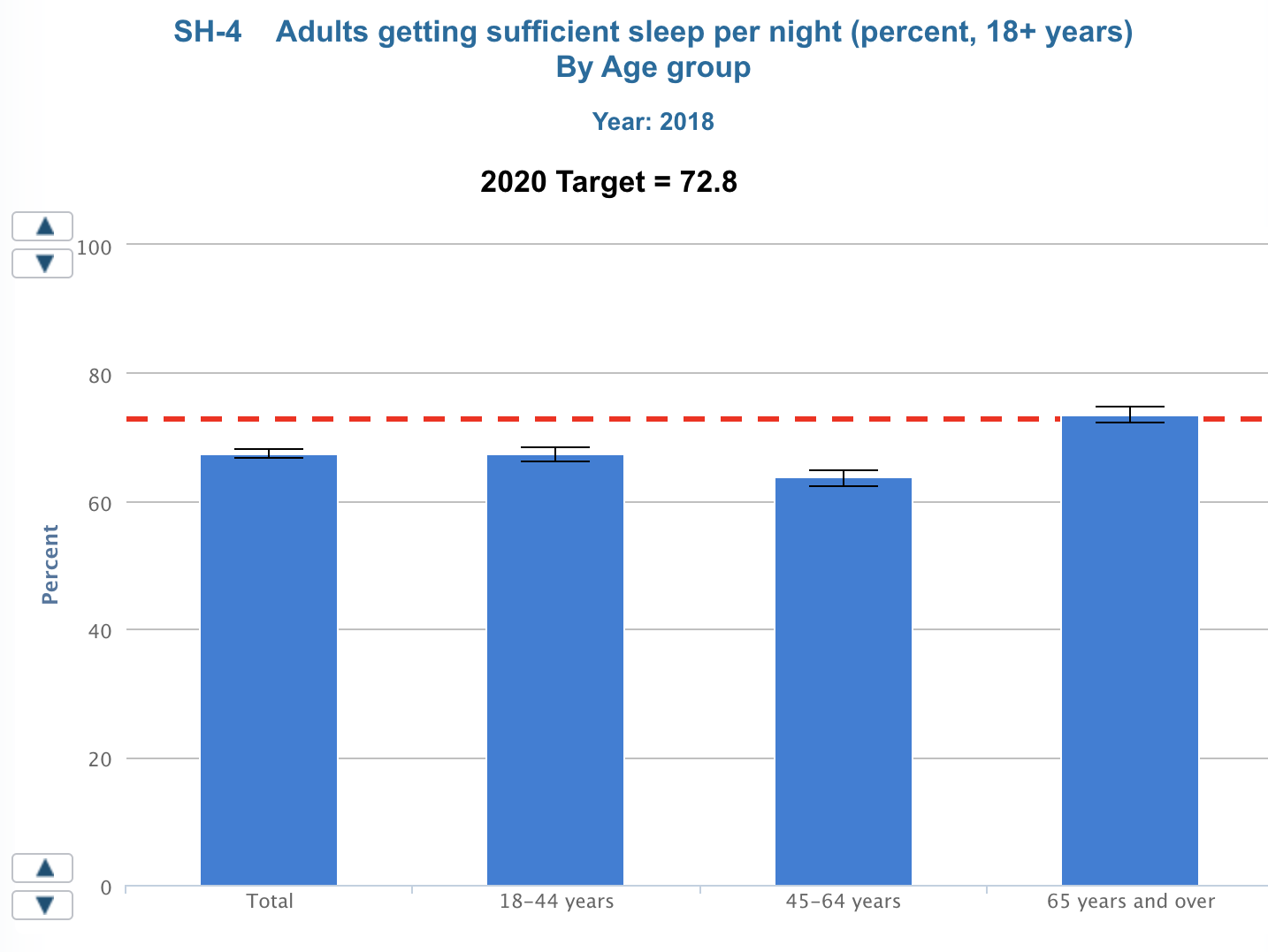
As for the Healthy People 2020 (2020) work to improve sleep health in the adult population, the key goal is to “increase public knowledge on how adequate sleep and treatment of sleep disorders improve health, productivity, wellness, quality of life, and safety on roads and in the workplace” (para. 1).
The goal covers four objectives targeted at the improvement of sleep health. First, it is expected to increase the number of patients with signs of obstructive sleep apnea who seek medical attention. Second, reducing the rate of vehicular crashes due to drowsy driving will improve the overall health and safety of the population. Third, the program should increase the number of students (grades 9 through 12) who get enough sleep. Fourth, the number of adults getting sufficient sleep should increase.
Interventions targeted at the improvement of sleep in adults are largely based on behavioral improvement efforts. For example, Kaar, Luberto, Campbell, and Huffman (2017) suggested mindfulness as well as other mind-body interventions as methods for improving a range of health outcomes, including sleep.
Such interventions are based on promoting muscle relaxation, meditation, yoga, and other mindful techniques that relax the body and mind, preparing an individual for a healthy and disturbance-free sleep (Kaar et al., 2017). Mindfulness interventions can also be used for the holistic treatment of insomnia and the improved physical activity in adults that leads to better sleep.
Redeker et al. (2019) suggested implementing employer-based interventions to improve sleep and its related outcomes among working adults. Employers who invest in the healthy rest of their workers usually have a workforce with better sleep habits and general fitness that facilitate increased performance in the workplace. Furthermore, better sleep means reduced absenteeism, which points to the need for employers to consider educational interventions for better sleep. In both interventions, data on adults’ sleep education, as well as the number of hours they sleep per night, should be collected.
To conclude, the Healthy People 2020 goal of improving sleep education as well as making sure that more adults get treatment for their sleep disorders intends to enhance the overall life quality in the population. Understanding sleep health and the adverse effect of sleep disturbances on the population’s health is imperative for reaching high levels of awareness of the problem as well as facilitating interventions that can address the main limitations of inadequate sleep and accompanying conditions.
References
Avidan, A. (2018). Review of sleep medicine. Philadelphia, PA: Elsevier.
Healthy People 2020. (2020). Sleep health. Web.
Kaar, J. L., Luberto, C. M., Campbell, K. A., & Huffman, J. C. (2017). Sleep, health behaviors, and behavioral interventions: Reducing the risk of cardiovascular disease in adults. World Journal of Cardiology, 9(5), 396-406.
Redeker, N. S., Caruso, C. C., Hashmi, S. D., Mullington, J. M., Grandner, M., & Morgenthaler, T. I. (2019). workplace interventions to promote sleep health and an alert, healthy workforce. Journal of Clinical sleep Medicine: JCSM: Official Publication of the American Academy of Sleep Medicine, 15(4), 649-657.